Social inequalities and their determinants
Social inequalities have long been observed and have an impact on health throughout the life course. Here, data broken down by determinants are presented as examples.
Gender
Single-parent families account for 25% of families in France, with women heading 80% of them, and they are more likely to face socio-economic hardship. Data from the 2021 Barometer show that these single mothers have experienced more major depressive episodes over the past year and smoke more daily than mothers in couples. Furthermore, single fathers are at greater risk of experiencing suicidal thoughts within the past year or of having attempted suicide at some point in their lives compared to fathers in couples with children.
According to the 2007–2010 Entred study, people with type 2 diabetes were predominantly men (55.3%), with an average age of 67.6 years; 76.3% were born in France, and 11.1% were born in a Maghreb country.
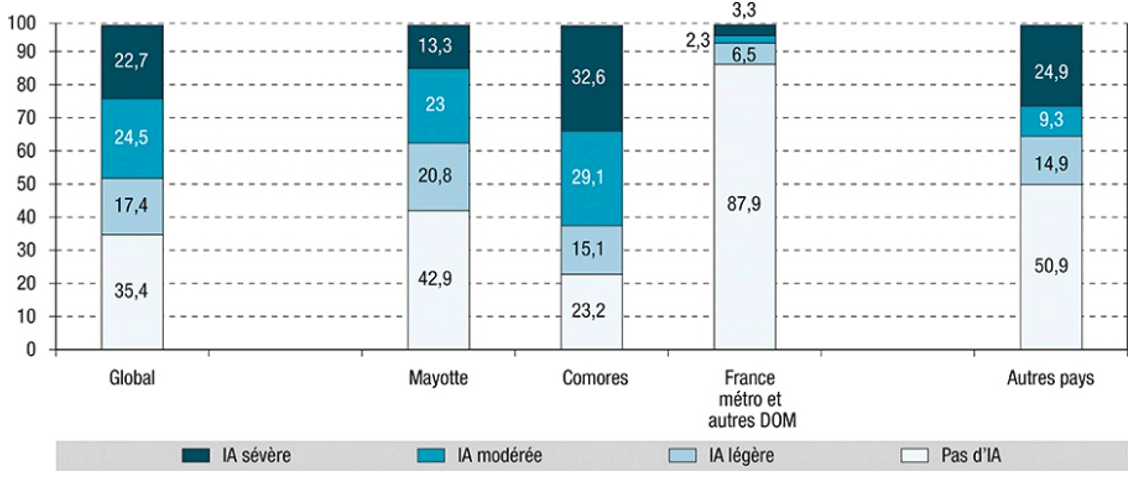
In 2019, according to the Unono Wa Maore study in Mayotte, nearly half of adults reported that their household was experiencing moderate (24.5%) or severe (22.7%) food insecurity. This prevalence varied significantly by place of birth; it was 36.3% among those born on the island, compared to 61.7% among those born in the Comoros. The lowest prevalence was 5.6% for those born in mainland France or other French overseas departments.
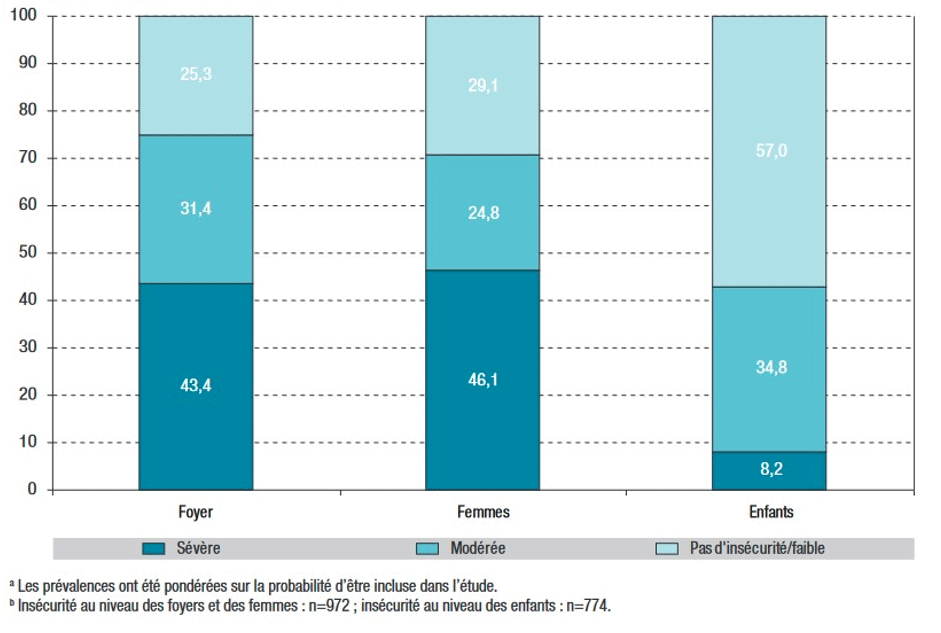
Of the 1,220 women included in the 2011–2012 Abena study, 972 were classified as experiencing food insecurity in their households or personally (79.7%). “Household-level” food insecurity was “severe” for 43%, “moderate” for 31%, and “absent or low” for one-quarter of them. Furthermore, 8% of women with children reported severe food insecurity for their children, and 35% reported moderate food insecurity.
Housing Conditions
Regarding the relationship between housing and health, the 2013–2014 Qualisurv-Habitat study, conducted among households living in substandard housing conditions, showed that respiratory health and mental health are, from the participants’ perspective, the two areas most affected by substandard housing conditions. Dampness and mold, energy poverty, and overcrowding are the most common issues, along with outdated electrical systems and structural instability.
The CoviPrev survey, conducted in 30 waves between March 2020 and January 2022, during the COVID-19 pandemic, shows that living in overcrowded housing (defined as less than 18 m² per person or less than 25 m² for a person living alone) increased the likelihood of experiencing depression, anxiety, and suicidal thoughts during the pandemic.
Learn more:
Du Roscoät E, Forgeot C, Léon C, Doncarli A, Pirard P, Tebeka S, et al. The mental health of the French population during the COVID-19 pandemic: key findings from surveillance and studies conducted by Santé publique France between March 2020 and January 2022. Bull Épidémiol Hebd. 2023; (26): 570-89.
Health in Action, September 2021, No. 457 - Housing, a major determinant of population health.
Working Conditions
Data from the Coset Covid-19 study conducted in 2020 during the COVID-19 pandemic highlighted the impact of occupational factors on health and health behaviors. In the aftermath of the lockdown, nearly 20% of women artisans, shopkeepers, and independent professionals suffered from anxiety, and 20% of women in independent professions exhibited depressive symptoms, though it was not possible to directly link these figures to the lockdown due to a lack of available baseline data. An increase in sleep difficulties was reported, particularly among non-agricultural self-employed individuals and agricultural workers. Certain occupational groups exhibited a higher prevalence of anxiety and depressive symptoms following the end of lockdown in June 2020, with the frequency of these symptoms appearing to be linked to unfavorable working conditions during lockdown.
Furthermore, data from the “Constances” cohort of the General Social Survey showed that work stoppages or changes in working hours during lockdown varied greatly across different socio-professional categories of employees, but were generally less frequent in this population than among non-agricultural self-employed individuals.
According to the 2021 Health Barometer, suicidal thoughts in the past 12 months were strongly associated with being unemployed, as well as with belonging to the “economically inactive” category, compared to those in the labor force. By employment status, the largest increase in characterized depressive episodes was observed among students (+7 percentage points), followed by the unemployed (+5.3 percentage points), employed individuals (+4.4 percentage points), and retirees (+1.7 percentage points). As in previous waves, the unemployed remained the most affected (22.0%) and retirees the least affected (7.5%) by a characterized depressive episode in 2021. Among both women and men, those who reported not being financially comfortable, living alone or in a single-parent household (compared to couples with children), as well as the unemployed (compared to employed individuals), were at greater risk of having experienced a major depressive episode during the year than others.
Learn more:
Léon C, du Roscoät E, Beck F. Prevalence of suicidal thoughts and suicide attempts among 18- to 85-year-olds in France: results from the 2021 Health Barometer. Bull Épidémiol Hebd. 2024; (3):42-56.
Léon C, du Roscoät E, Beck F. Prevalence of depressive episodes in France among 18- to 85-year-olds: results from the 2021 Health Barometer. Bull Épidémiol Hebd. 2023;(2):28-40.
Social Disadvantage
As of January 1, 2020, the prevalence of treated epilepsy was estimated at 10.2 per 1,000 inhabitants in France (source: SNDS). The prevalence, which is similar among men and women, increases with age and rises steadily with social disadvantage. There is regional variation in treated epilepsy, with higher prevalence in northern departments and those located along a northeast-southwest diagonal, as well as in certain overseas departments.