Health Issues
Social and Regional Health Inequalities: Health Challenges
In France, the population’s health status is marked by a paradox: good health on average, but significant social health inequalities beginning in childhood and continuing throughout life. By hitting the most disadvantaged populations hardest, the COVID-19 pandemic has brought home to the general public the impact of social determinants on people’s health.
What are social inequalities in health?
According to the World Health Organization, social inequalities in health are significant and systematic differences in health status observed between social groups. These inequalities are not due to chance or biological factors, but are socially constructed and reflect injustices in the distribution of resources and opportunities. They are socially constructed and can manifest according to characteristics (gender and sexual orientation, etc.) or a social gradient (income disparities, education level, occupation, etc.). They are the result of inequitable living conditions, where certain groups have less access to the healthcare system, education, decent housing, secure employment, or a healthy environment.
What factors influence health?
According to the World Health Organization’s definition, health determinants are the “personal, social, economic, and environmental factors that determine the health status of individuals or populations.” They contribute to the development of social inequalities in health.
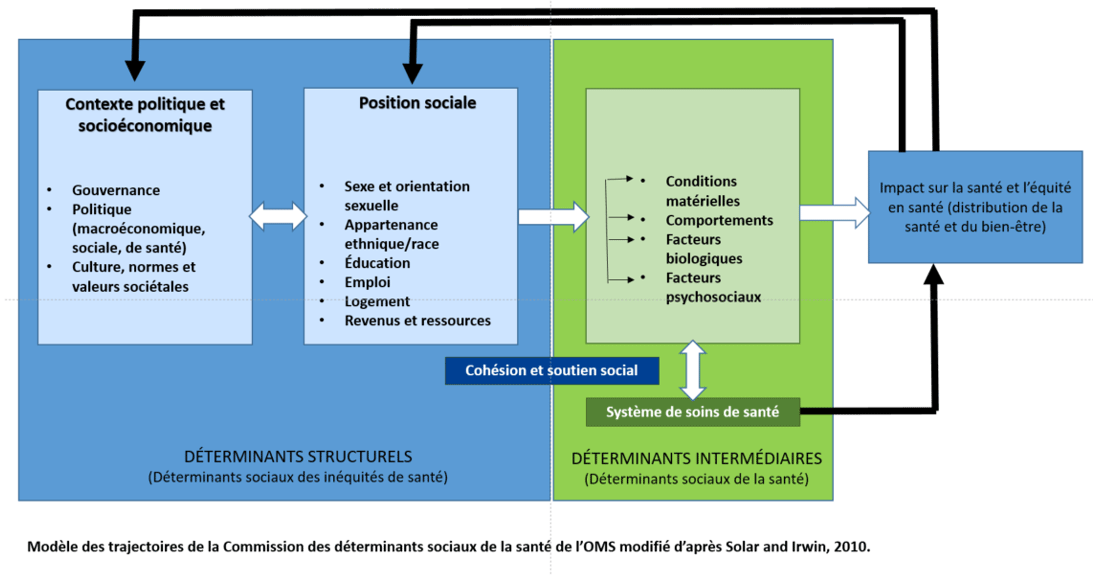
At every stage of life, health status is characterized by complex interactions among various socioeconomic factors, which are interdependent with the physical environment and individual behavior. These factors, referred to as “determinants of health,” are classified as structural and intermediate determinants. They do not act in isolation: it is the combination of their effects that influences health status.
Environmental determinants of health in the broadest sense include not only physical, chemical, and biological factors external to an individual, but also living conditions and the social environment. These environmental threats may result from social conditions and individuals’ lifestyles. Environmental determinants include water, air, and soil quality, as well as the quality of housing, living conditions, food, and so on. These may include exposure to chemical risks such as pesticides, metals (lead and mercury), and other pollutants (persistent pollutants, nanoparticles, microplastics), as well as exposure to climate change (extreme temperatures, wildfires, floods) and the emergence of new environmental risks (e.g., electronic waste).
These determinants often have a disproportionate impact on children and pregnant women. Social health inequalities arise and widen as early as pregnancy and the first years of life, particularly due to the socially differentiated exposures of the mother and living conditions during this period. However, in early life, children are particularly sensitive to their environment (psycho-emotional, physical, and chemical), which can have a specific influence on their genes and may or may not promote the development of certain chronic diseases, such as obesity or diabetes (see https://www.1000-premiers-jours.fr/fr).
So-called “structural” determinants depend on a country’s political, cultural, economic, and social structures. These determinants encompass the nature and scope of values, beliefs, worldviews, culture, and norms; governance; laws, policies, regulations, and budgets; and institutional practices, and they determine the social position occupied by individuals.
Learn more: Keeping it political and powerful: Defining the structural determinants of health | National Collaborating Centre for Determinants of Health
Structural determinants of health produce (or result in) inequalities that are expressed (or observed) primarily in terms of:
Gender
Background (country of birth, biological and genetic heritage)
Level of education, schooling, literacy
Income and resources
Employment
Housing and surroundings (basic amenities, safety, health-promoting urban design)
Social inclusion/social support and non-discrimination, (absence of) violence
Access to and use of affordable, high-quality health services
Structural determinants influence the health of individuals (or populations) through intermediate determinants.
So-called "intermediate" determinants are the consequences of structural determinants. These include living and working conditions, health behaviors (such as alcohol and drug use, nutrition, and emotional and sexual life), biological factors, and psychosocial factors.
Which groups are most affected by social inequality?
Data show that the lower an individual’s socioeconomic status, the poorer their health.
Living and working conditions in the broadest sense can be undermined by discrimination and prejudice, which most often affect women and girls, older adults, people with disabilities or health conditions (particularly mental health issues), people of foreign origin, or people whose behaviors or culture differ from the dominant social norm (sexual orientation, drug users, gender identity, socially marginalized populations).
We also identify populations excluded from the healthcare system, which include a diverse range of people more likely to lack access to the resources, goods, or services enjoyed by the majority, due to their living conditions—particularly material ones—their socio-economic vulnerability, and their social position (lack of access to housing, employment, education, income, or administrative status).
For certain populations, experiences of social exclusion are compounded by the inability to exercise social rights (Source: National Council on Policies to Combat Poverty and Social Exclusion). These socially excluded individuals are more likely to be unable to assert their social rights, and for some, language barriers, a lack of social support, and low health literacy prevent them from accessing the healthcare system.
Focus on Regional Health Inequalities in France
Living conditions, working conditions, and mobility, as well as access to health, cultural, and recreational facilities and services, are not uniform across France. The departments with the lowest standard of living are located in the north, the center, along much of the Mediterranean coast, and in the overseas departments and regions (DROM), while the wealthiest households are concentrated in areas bordering Switzerland, as well as in most major metropolitan areas. From a territorial perspective, healthcare professionals are unevenly distributed not only across municipalities but also across departments and entire regions (Source: INSEE).
Environmental differences, such as exposure to pollutants and vector-borne diseases, also contribute to health disparities. These differences are particularly evident between urban and rural areas and between overseas territories and mainland France; they are exacerbated by climate change. Furthermore, the most socially disadvantaged urban areas are at greater risk of being environmental hotspots, which are areas with the highest cumulative overexposure to heat, air pollution, and lack of vegetation. These results are not observed in rural areas, which can likely be explained by a more diffuse and heterogeneous distribution of social disadvantage and less granular spatial scales than in urban areas.
Learn more:
Certain regions are more vulnerable to health crises due to their level of poverty, high population density, limited availability of healthcare facilities and services, or increased exposure to environmental risks. In recent years, the consequences of extreme weather events have become increasingly frequent and intense due to climate change. The DROMs, in particular, are among the French territories most exposed to the impacts of this phenomenon, due to their coastal location and the fragility of their ecosystems.
The Case of the Drinking Water Crisis in Mayotte
By the end of January 2023, rainfall was 40% lower than in a typical year in certain areas of Mayotte, particularly those home to the two hillside reservoirs that account for approximately 80% of the department’s water supply. Water shortages expose the population to increased health risks, especially since a large portion of Mayotte’s residents live in precarious conditions (77% of the population lives below the national poverty line). The lack of water supply can lead to:
the use of water unfit for consumption;
insufficient hydration;
an inability to practice basic hygiene, including handwashing;
poor sanitation and the inability to dispose of waste;
the storage of water unfit for consumption or likely to serve as breeding grounds (for mosquitoes).
Learn more - Drinking water crisis in Mayotte: enhanced measures in response to the exceptional situation (news from 11/29/23)