Data
Sleep Duration
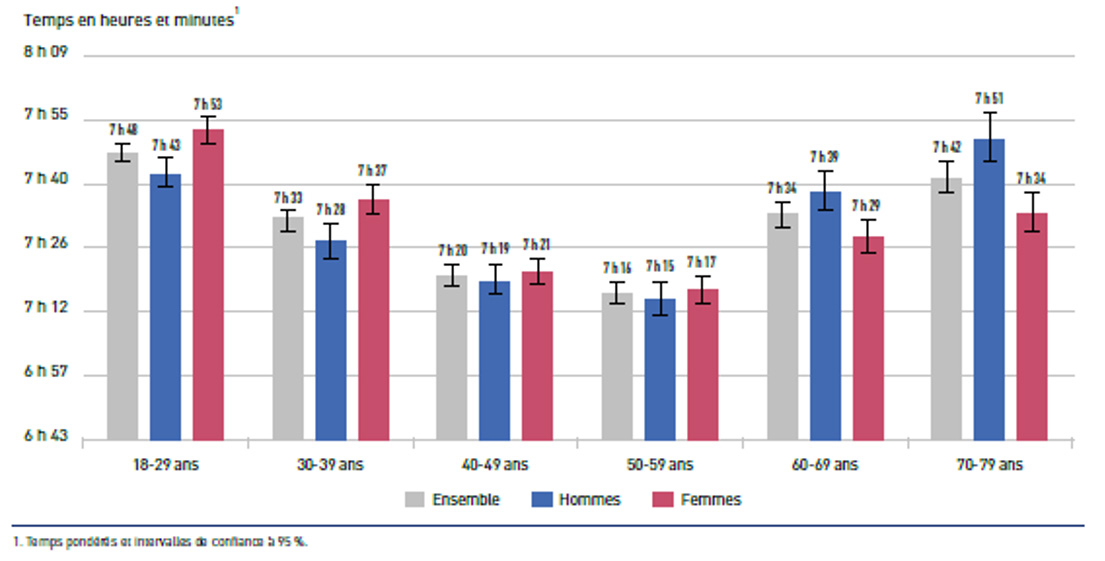
In 2024, according to the Santé publique France survey, the average sleep duration over a 24-hour period is 7 hours and 32 minutes among adults aged 18–79, with significant variations by age and gender.
People aged 50 to 59 have the shortest average sleep duration (7 hours and 16 minutes), while those in the extreme age groups (18–29 and 70–79) have the longest sleep durations. Among women, average sleep duration is highest among those aged 18–29 (7 hours and 53 minutes), whereas among men, it is highest among those aged 70–79 (7 hours and 51 minutes).
Average sleep duration thus decreases as financial difficulties increase, dropping from 7 hours and 38 minutes for those who are financially secure to 7 hours and 22 minutes for those in difficult financial situations or in debt. This situation can be explained, among other things, by:
- greater mental health vulnerability, as shown by studies on depression and anxiety,
- living conditions that are unfavorable to quality rest: noise pollution, lack of privacy, exhausting daily commutes, or an unsafe living environment.
Short sleepers
In 2024, according to the Santé publique France survey, 21.5% of people aged 18–75 are considered short sleepers, with marked disparities based on factors such as gender, age, family situation, socioeconomic status, and geographic location:
men (22.4%) are more affected than women (20.6%),
people aged 50–59 are the most affected (26.1%) compared to those at the older and younger ends of the age spectrum,
25.6% of people in single-parent households are short sleepers, compared to 17.7% of childless couples,
the proportion of short sleepers rises from 15.4% among those who are financially comfortable to 29.0% among those in financial difficulty,
24.3% of those without a high school diploma are affected; this figure rises to 27.0% among manual laborers,
the French overseas departments in the Americas (Guadeloupe, Martinique, French Guiana) have over 30% of short sleepers,
in mainland France, the Île-de-France region has a high rate (24.1%), while the Pays-de-la-Loire, Brittany, and Nouvelle-Aquitaine regions have the lowest proportions.
It is worth noting that short sleepers face an increased risk of being overweight, obesity, type 2 diabetes, high blood pressure, cardiovascular disease, depression, or accidents—even if potential daytime naps help partially compensate for possible sleep deficits at night.
Learn more:
Itani O, Jike M, Watanabe N, Kaneita Y. Short sleep duration and health outcomes: a systematic review, meta-analysis, and meta-regression. Sleep Med. 2017 Apr;32:246-256.
Faraut B, Touchette E, Gamble H, Royant-Parola S, Safar ME, Varsat B, Léger D. Short sleep duration and increased risk of hypertension: a primary care study.
Complaints of insomnia
In 2024, according to the Santé publique France barometer, one-third of adults aged 18 to 79 (33.1%) reported insomnia, with significant variations by gender, age, socioeconomic status, and geographic location:
women are more affected (37.7%) than men (28.2%),
among men, just over 25% of those aged 18–49 are affected, compared to about 30% of those aged 50–79,
among women, 31.7% of those aged 18–29 report insomnia, compared to 43.4% of those aged 70–79,
45.8% of people experiencing financial difficulties, 37.9% of those without a high school diploma, and 38.8% of employees are affected,
the highest rates are observed in Guadeloupe (38.5%), French Guiana (38.3%), and Réunion (39.4%).
Women's Sleep
According to the 2024 Santé publique France survey, women aged 18 to 29 report sleeping an average of 10 minutes longer than men of the same age. Between the ages of 70 and 79, the trend reverses: they sleep 17 minutes less than men. This decline in sleep duration with age is accompanied by an increased frequency of insomnia complaints, affecting 43.4% of them. At all ages, they report more insomnia problems than men.
Several factors, often intertwined, explain these disparities:
biological causes: such as hormonal changes (menstrual cycles, menopause) that disrupt sleep,
psychological factors, such as a higher prevalence of anxiety and depression,
societal pressures, particularly greater involvement in household chores and family responsibilities, contribute to impairing the quality of their sleep.
Sleep Among 11- to 17-Year-Olds
In 2022, according to the EnCLASS survey, among psychological and physical complaints experienced more than once a week over the past six months, difficulty falling asleep was the most common among middle school students (43.0%) and high school students (42.2%), ahead of nervousness (36.6% and 45.4%, respectively) and irritability (34.3% and 39.6%, respectively). Difficulty falling asleep is reported more frequently by girls (49.9% in middle school and 50.8% in high school) than by boys (36.4% and 33.5%).
Furthermore, the study of depressive symptoms, assessed using the ADRS (Adolescent Depression Rating Scale), showed that one-third of adolescents (34.2% of middle school students and 34.5% of high school students) reported sleeping very poorly; with a higher proportion among girls (42.9% in middle school and 42.8% in high school) than among boys (25.9% and 26.2%).
Chronic insomnia
In 2017, 13.1% of people aged 18–75 reported symptoms suggestive of chronic insomnia, 16.9% of women and 9.1% of men (p<0.001). Chronic insomnia was more common among women aged 25 to 64 (around 19%) and among men aged 35 to 64, affecting about one in 10 men. Regardless of age, women were about twice as likely as men to report symptoms of chronic insomnia.
Heavy daily smokers were significantly more likely to suffer from chronic insomnia than other smokers or nonsmokers (25.5% vs. 12.6%, p<0.001). Tobacco is a cofactor associated with “short sleep,” insomnia (among daily alcohol users), and the evening chronotype. It therefore deserves to be taken into account in studies linking sleep and cardiovascular indicators. This link between smoking and sleep quality should encourage smokers to quit. Alcohol or illicit drug use did not show a significant difference regarding chronic insomnia.
Napping
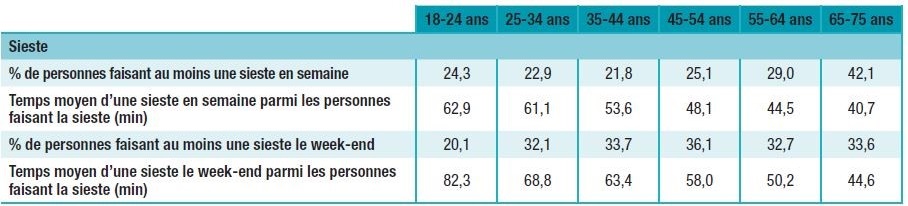
In 2017, more than a quarter of French adults aged 18 to 75 reported taking a nap at least once a week, lasting an average of 50 minutes, and nearly a third of them reported taking a nap at least once on the weekend, lasting an average of 1 hour. Recovering sleep on the weekend appears to be a factor that reduces the risk of comorbidities associated with short sleep duration. The ability to make up for sleep debt on the weekend can therefore also be viewed as a positive factor.
Indicators on napping during the week and on weekends, by age. Santé publique France Barometer 2017
The Impact of Stress on Sleep
In 2017, half of French people (48%), mostly women (56%) and those in lower socioeconomic classes (56%), reported experiencing stress that significantly affected their sleep. Those who described themselves as very stressed were the ones who slept the least during the week (6 hours or less). Women, who are more prone to stress due to a combination of factors (physiology, social roles, the mental burden of family and their well-being, and the rise of single-parent families), experienced more fragile sleep.
Sleep Disorders
In 2017, a high proportion of French people suffered from sleep disorders, the most common of which are insomnia (15–20% of adults), sleep apnea syndrome (4–6% of adults), restless legs syndrome (2% to 8% of the population), parasomnias (2–4%), and rare hypersomnias (0.05% to 0.1% of the population).
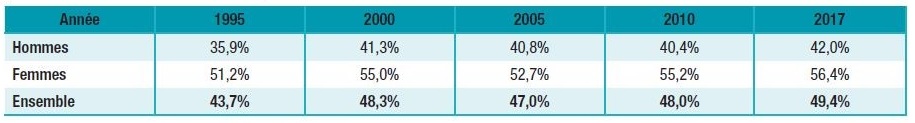
Changes in the proportion of people reporting sleep problems over the past 8 days, between 1995 and 2017, by gender and among those aged 18–75
Sleep: The Second-Biggest Health Concern in 2024
According to the results of the exploratory study conducted in 2024, 44% of respondents rank sleep as their second-biggest health concern, while 55% of those who rate their sleep as poor or very poor cite it as their top concern. More broadly, 61% of respondents say they are dissatisfied with their sleep, and 79% report regular sleep disturbances.
The main obstacles cited are stress, demanding schedules, family life, and resignation in the face of external factors that hinder the adoption of best practices. Women, shift workers, and parents are particularly vulnerable.
Although adults are generally well-informed, they struggle to follow recommendations (reducing screen time, physical activity, regular schedules, consulting a professional). Persistent barriers to change include a lack of support, a sense of ineffectiveness, and the perception of sleep as an individual and complex issue.
The quantitative study reveals five distinct types of behavior:
the exemplary: naturally follow best practices and sleep well,
the optimizers: active and connected, but sometimes at the expense of their sleep,
the vulnerable: stressed and resigned after having tried everything without success,
the resigned: fatalistic, reluctant to take action to improve their situation,
the experimenters: motivated to try out solutions, despite feeling they lack information.
Sleep During the COVID-19 Pandemic
During the COVID-19 period, results from the CoviPrev survey by Santé publique France revealed a lasting decline in sleep quality among the French population. Thus, by mid-January 2022, sleep problems affected 66% of respondents. This prevalence indicated a structural increase, as the rate was significantly higher than the level observed outside the pandemic in 2017, which stood at 49%. The severity of these sleep disturbances even exceeded that recorded at the start of the first lockdown in March 2020, when it reached 61%. Sleep disturbances affected particularly vulnerable populations, notably women, unemployed individuals facing financial difficulties, and those aged 18–24.