Data
Approximately 175,000 people were treated for Parkinson’s disease in France in 2020
A method developed by Inserm in partnership with Santé publique France makes it possible to identify people treated for Parkinson’s disease using reimbursement data for anti-Parkinson’s medications available in the National Health Data System (SNDS1). This makes it possible to estimate the prevalence of Parkinson’s disease.
In 2020,
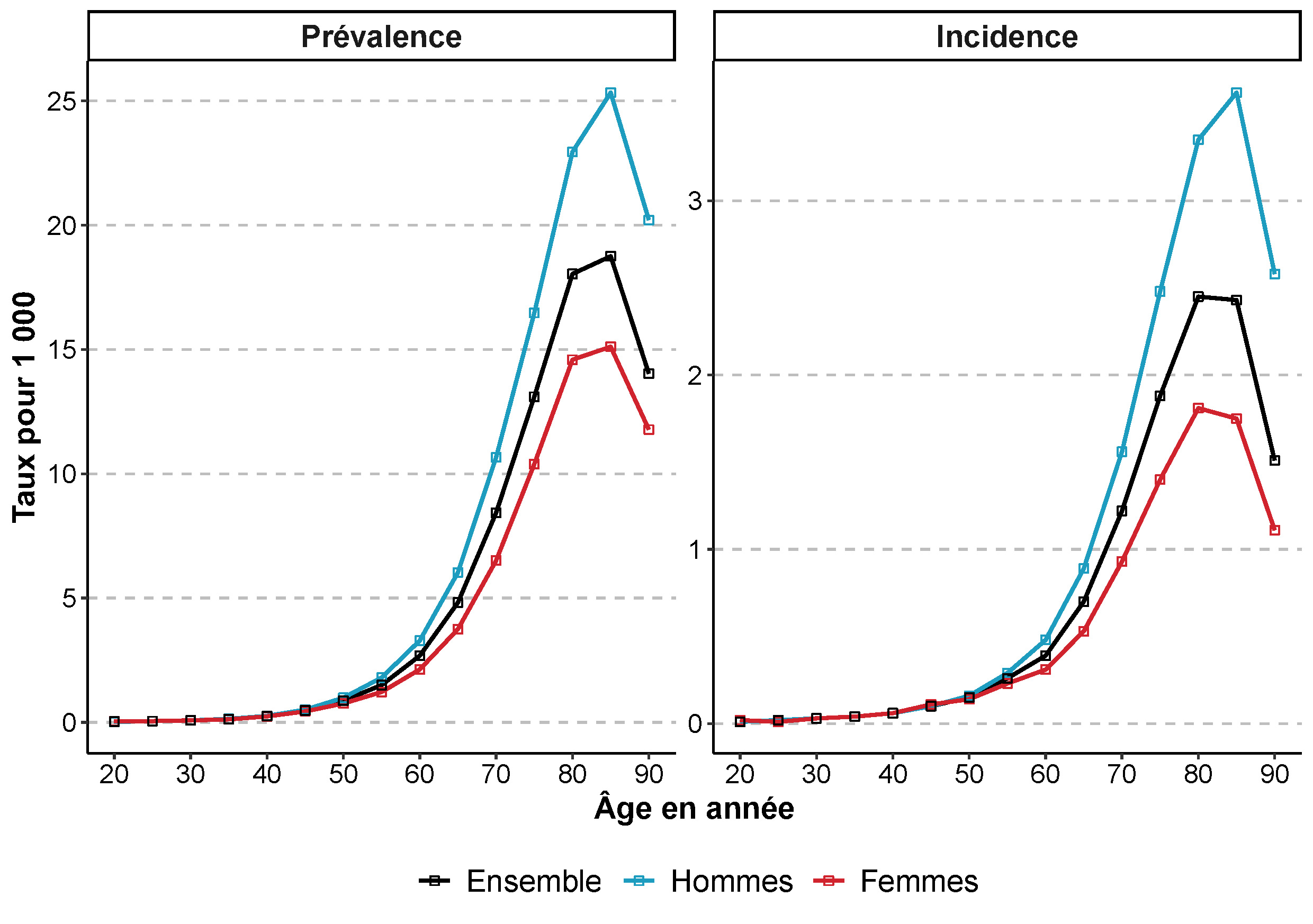
approximately 175,000 people were treated for Parkinson’s disease in France, representing a prevalence of 2.63 per 1,000 inhabitants.
With nearly 26,000 new patients treated in 2020, the annual incidence was estimated at approximately 0.38 new cases per 1,000 people.
The average age of patients at the start of treatment was 75 years.
Parkinson’s disease is about 1.5 times more common in men than in women.
|
|
Age-standardized prevalence rate |
Age-standardized incidence rate |
|---|---|---|
|
Men |
3.35 per 1,000 people |
0.51 per 1,000 person-years |
|
Women |
2.11 per 1,000 |
0.29 per 1,000 person-years |
The prevalence of Parkinson’s disease increases sharply with age; it rises steadily among people aged 50 to 80, peaks between the ages of 85 and 89, and then declines. This decline may be due to underreporting of cases among the oldest patients.
These data, along with those from 2010 to 2020, are available at the following address: https://dataviz.santepubliquefrance.fr/parkinson/
A Growing Burden
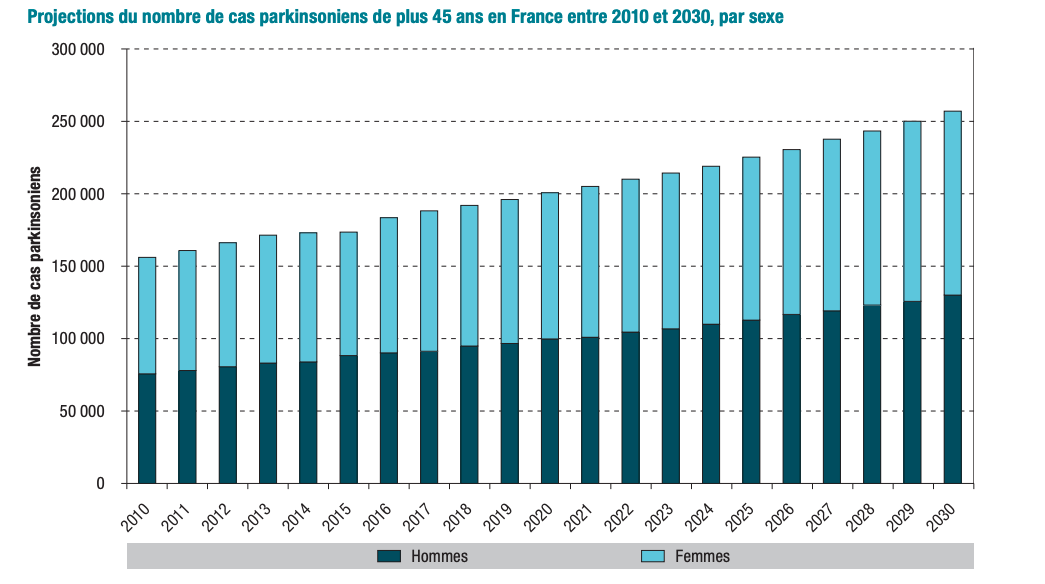
In collaboration with the biostatistics team at Inserm Unit 1219, we estimated, assuming a constant annual incidence (i.e., a constant number of new cases each year), that the number of people with Parkinson’s disease will increase by 56% in 2030 compared to 2015, with one in every 120 people over the age of 45 affected by 2030. This increase is mainly due to population aging and the longer duration of the disease.
Nearly 75,000 people were hospitalized in 2012
This indicator describes hospital admissions for Parkinson’s disease in France among people aged 40 and older, regardless of their health insurance coverage. It can be broken down by age, sex, region, and different hospital settings: medicine, surgery, and obstetrics (MCO), follow-up care and rehabilitation (SSR), home hospitalization (HAD), and psychiatry.
The number of people aged 40 and older hospitalized in 2012 with a diagnosis of Parkinson’s disease, regardless of the primary reason for hospitalization, totaled 74,454 (38,734 men and 35,720 women), representing 47% of prevalent cases: 66,119 patients were hospitalized in general medical care (for a total of 101,755 stays), 22,645 in SSR, 1,891 in HAD, and 812 in psychiatry.
92% of hospitalized patients are over 65 years old and 55% are over 80 years old. The median age at the time of hospitalization is 81 years, with no significant difference between men and women.
A disease associated with reduced life expectancy
Between 2009 and 2015, we followed a cohort of over 130,000 people who developed Parkinson’s disease; the maximum follow-up period for patients was 7 years, and the average follow-up was 3.5 years. We were thus able to estimate, for the first time in France, the survival and mortality indicators associated with this disease by sex and age group:
During the follow-up period, nearly a quarter of patients died. The average age at death was 83.3 years.
The 5-year survival probability is approximately 60% for men and 70% for women. More than 90% of deaths occur after age 70.
People with Parkinson’s disease have a risk of death that is twice as high as that of healthy individuals of comparable age and sex.
This increased risk of death for people with Parkinson’s disease compared to those without the disease is more pronounced among younger patients and women.
Documented causes of death
Our study, based on the CépiDc-Inserm2 medical cause-of-death databases, identified and characterized individuals aged 50 and older who died with Parkinson’s disease in France in 2014 and documented the causes of their deaths.
Among nearly 500,000 deaths reported in 2014 among individuals aged 50 and older, approximately 2% mentioned Parkinson’s disease.
Parkinson’s disease was the underlying cause of death for 58% of those who died with a mention of this disease on their death certificate, with comparable rates among men and women. The other primary causes of death were (in descending order of frequency):
Diseases of the circulatory system: 14%
Invasive neoplasms: 6%
Alzheimer’s disease and other dementias: 4%
Falls and other external causes: 4%
Respiratory diseases: 3%.
French regions affected to varying degrees
The geographic distribution of Parkinson’s disease shows regional disparities. These are difficult to interpret, as regions may differ from one another in many ways: environment, organization of the healthcare system, population, and so on. Furthermore, since the method for identifying Parkinson’s patients relies on healthcare reimbursement data, these disparities may also reflect differences in care management or access to healthcare across regions.
Regional and departmental data are available on the Géodes platform.
Studies on the association between Parkinson’s disease and agricultural activities
Santé publique France has conducted several studies in collaboration with Inserm Unit 1018 on the relationship between agricultural characteristics or occupational exposure to pesticides and Parkinson’s disease:
A study conducted in partnership with Inserm2 and the Mutualité sociale agricole (MSA1) among MSA1 members in five departments (Charente-Maritime, Côte-d’Or, Gironde, Haute-Vienne, Mayenne) found in 2007 an increase in the prevalence of Parkinson’s disease of approximately 25% among MSA1 members in cantons characterized by the highest densities of orchards specializing in fruit (apples, pears, cherries, apricots, plums, and peaches) and other perennial crops (lemons, kiwis, nuts, blackcurrants, raspberries, etc.).
A case-control study compared pesticide use (assessed via questionnaire) among 133 farmers with Parkinson’s disease to that of 298 farmers without the disease. Those with the disease reported more frequently than others having been exposed to pesticides on farms specializing in viticulture. The strongest associations were found for occupational exposure to insecticides and fungicides, particularly among farmers who had used these substances for a long time.
A study describing the incidence of Parkinson’s disease among MSA1 members (2011–2012) observed a higher incidence of the disease among this specific population, particularly among farmers (+13%) compared to the rest of the French population.
A study also describing the incidence of Parkinson’s disease among MSA members (2010–2015) observed an increase in incidence among this specific population in geographic areas where annual pesticide expenditures by farms specializing in non-appellation viticulture were highest.
These findings underscore the need to continue epidemiological surveillance of Parkinson’s disease among the agricultural population and help identify situations—particularly occupational ones—that may pose a risk for Parkinson’s disease and where specific research should be encouraged.
These results, along with those produced by other French and international organizations, contributed to the recognition in 2012 of Parkinson’s disease as an occupational disease for farmers who have performed work involving regular exposure to pesticides for at least 10 years (Table 58 of the agricultural scheme).
We extended this study to cover the entire metropolitan area for the period 2010–2012—which accounts for more than 90% of the French population—and found an increase in the incidence of Parkinson’s disease (+11%) among people living in cantons where the proportion of agricultural land allocated to viticulture is highest, compared to those living in cantons where this proportion is lowest; this association was also found in analyses that did not account for farmers. These results suggest that environmental exposure to pesticides may also be associated with an increased risk of Parkinson’s disease and that the number of Parkinson’s disease cases attributable to pesticides may be higher than if occupational exposure alone were involved. Further studies are still needed in this area to better understand and characterize this relationship.
See also

National Health Data System (SNDS): a medical-administrative database containing health care services covered by the National Health Insurance (doctor visits and medical procedures, medications, hospitalizations, etc.), medical causes of death, and a sample of data from supplemental health insurance providers. The data is linked while ensuring the anonymity of individuals.
data
Access national, regional, and county-level data
Prevalence of Parkinson's disease from 2010 to 2020
Geodes
Follow the latest developments regarding Parkinson's disease in France and in your region