The disease
Lead Poisoning in Children
Lead poisoning in children is the poisoning of a child by lead. Still prevalent in France, lead poisoning in children can have serious consequences for children. As such, lead poisoning in children is a reportable disease. In this context, Santé publique France’s priorities are to ensure the epidemiological surveillance of lead poisoning as well as its screening.
Lead has no known physiological role in humans. Its presence in the body therefore always indicates contamination. Lead absorbed through the digestive, respiratory, or bloodstream (mother-fetus) is distributed into the blood, soft tissues, and especially the skeleton (94%), where it gradually accumulates and remains stored for a very long time (half-life >10 years).
Serum lead levels (lead concentration in the blood) measured in venous blood are the indicator used to assess lead exposure. Serum lead levels reflect a specific state of equilibrium between an ongoing contamination process, the storage or release of bone lead, and elimination (excretion, skin, sweat). After the cessation of a poisoning process, blood lead levels decrease with a half-life of 20 to 30 days until a new equilibrium is reached, the level of which depends on bone stores. Blood lead levels are generally expressed in micrograms per liter (µg/L).
Young children are particularly vulnerable to poisoning because they ingest lead more frequently due to their hand-to-mouth behavior, have a high rate of intestinal absorption, and are in the developmental stage of their nervous system.
A case of lead poisoning in children is defined based on blood lead levels. Since June 2015, a case has been defined as a person under 18 years of age whose blood lead level reaches or exceeds the threshold of 50 µg/L (previously 100 µg/L).
For Santé publique France, the challenge is to monitor epidemiological data on childhood lead poisoning and its screening in order to identify and reduce the risks of lead exposure.
Sources of lead exposure
The main sources of lead exposure in children are:
Dust and flakes of lead-based paint (“white lead paint”) found in homes built before 1975, and especially those built before 1949
Tap water contaminated by lead pipes
Occupational or recreational activities engaged in by the child’s family or the child themselves: stained-glass restoration, foundry work, the manufacture of ceramics, enameled objects, ammunition, or lead objects (toy soldiers, etc.), battery recycling, metalwork, sport shooting, etc.
Handcrafted tableware (tagine dishes, ceramics, crystal, pewter), traditional cosmetics (kohl, surma), or traditional remedies ingested or applied to mucous membranes or wounds (azarcon, greta)
Recent travel to or regular stays in high-risk geographic areas, such as Africa, Madagascar, India, Pakistan, China, the Middle East, South America, or certain Eastern European countries (contaminated soil, traditional tableware, toys, food, etc.)
Soil contaminated by current or past industrial or mining activities (smelters, storage sites, auto junkyards, battery recycling facilities)
Exposure to tobacco smoke in the home (secondhand smoke)
In utero exposure, in the case of a pregnant woman with lead poisoning (during pregnancy or due to the release of lead from bones following past exposures).
See also
A condition with nonspecific symptoms
Low-level lead poisoning does not result in specific symptoms or clinical signs and often goes unnoticed. Only through proactive efforts to identify risk factors for a child’s exposure, followed by ordering a blood lead level test when such factors are identified, can lead-poisoned children be detected.
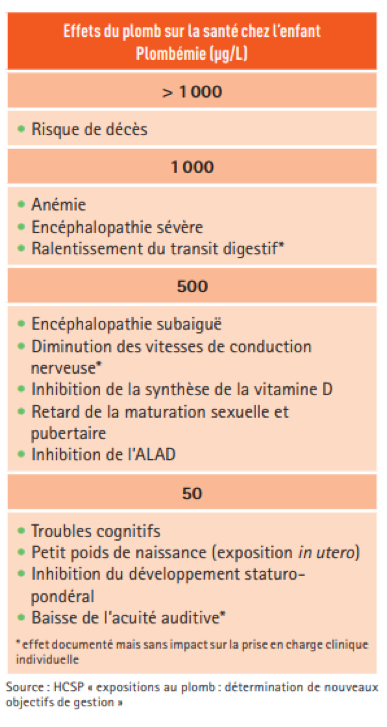
The health effects of lead poisoning, which are proportional to exposure, are variable and delayed. However, even at low concentrations, lead exposure already has serious consequences for a child’s psychomotor development.
Blood lead levels below 50 µg/L can cause damage to the central nervous system, including a decline in certain cognitive functions or learning abilities, which are irreversible.
In pregnant women with lead poisoning, there is a risk of miscarriage, premature birth, or gestational hypertension.
At birth, the infant’s blood lead level, measured in the umbilical cord blood, is similar to that of the mother.
Management: A Balance Between Monitoring and Intervention
The guidelines for screening and management of lead poisoning in children and pregnant women are outlined in the updated practical guide to screening and management of lead exposure in minors and pregnant women, published in 2017 by the High Council for Public Health.