Data
The surveillance system for vascular diseases of pregnancy established by Santé publique France enables the analysis of various epidemiological indicators.
Prevalence of cardiovascular and cerebrovascular diseases in women during pregnancy
Mortality
According to the report of the confidential national survey on maternal deaths published by the National Expert Committee on Maternal Mortality in January 2024, cardiovascular diseases are:
one of the top two causes of maternal mortality in France in 2016–2018 when considering all deaths occurring up to one year after childbirth;
the leading cause of maternal mortality when the postpartum period is defined as the 42 days following childbirth.
This report highlights that 56% of the 41 identified maternal deaths were considered preventable, with suboptimal care in 57% of cases, indicating room for improvement, particularly in the cardiovascular field and associated risk factors.
Strokes and Acute Coronary Syndromes (ACS)
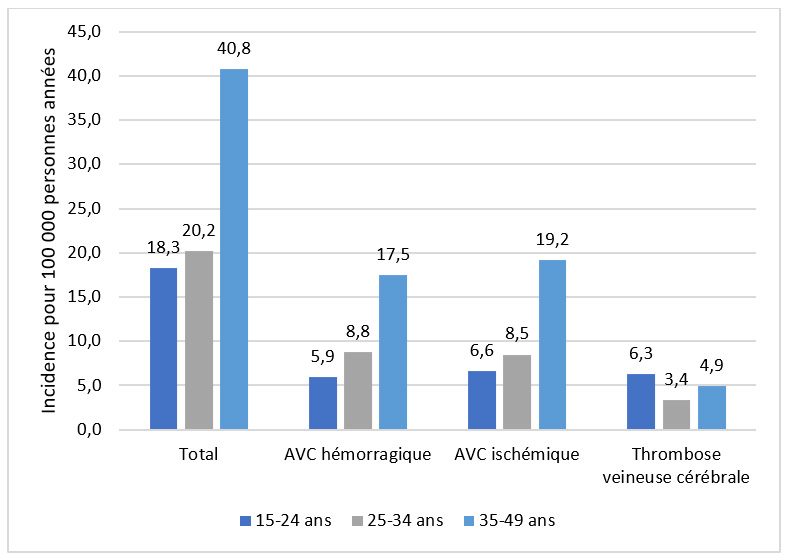
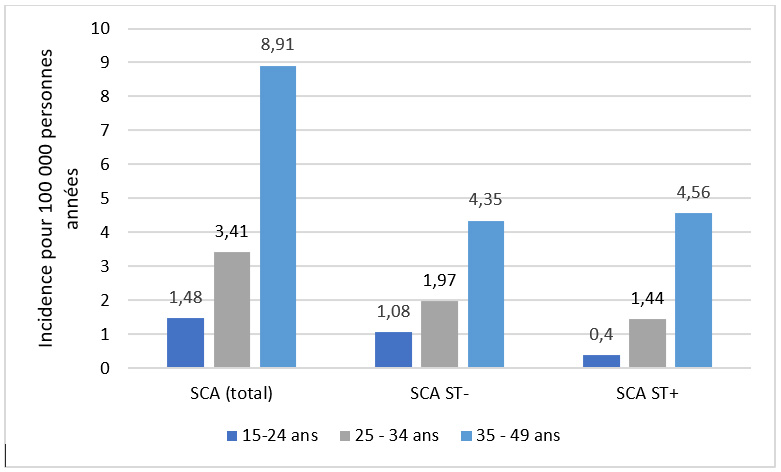
Data from the CONCEPTION cohort show that the incidence of strokes and ACS during pregnancy was 1 in 5,000 and 1 in 23,000 pregnancies, respectively, with a particularly high incidence in the period surrounding childbirth (the peripartum period) and the 6 weeks following childbirth (postpartum). One-third of ACS and stroke cases occurred during pregnancy, and two-thirds during the peripartum and postpartum periods.
Strokes during pregnancy exhibited some distinct characteristics, with an increased risk of hemorrhagic strokes and cerebral venous thrombosis compared to non-pregnant women of the same age.
The age-adjusted incidence of strokes during pregnancy and the postpartum period increased by 35% between 2010 and 2018, while that of ACS remained stable.
Heart Failure
According to the 7th Confidential Inquiry into Maternal Deaths, cardiovascular diseases are the leading cause of maternal mortality within 6 weeks of delivery, with heart failure and cardiomyopathies being the conditions most frequently implicated in these deaths.
In the CONCEPTION cohort, the incidence of heart failure is 35.6 cases per 100,000 pregnancies, or 1 case per 2,808 pregnancies. Only 22.6% of these women have a known history of heart disease identified in the SNDS, primarily cardiomyopathies and valvular heart diseases.
Pregnancies marked by an episode of heart failure are more frequently multiple, achieved through assisted reproductive technology, and complicated by gestational diabetes or hypertensive disorders, particularly preeclampsia. Women hospitalized for heart failure during pregnancy or the postpartum period are significantly older and suffer more frequently from hypertension and obesity.
Venous Thromboembolic Disease (VTE)
In 2013, the incidence of hospitalizations for deep vein thrombosis or pulmonary embolism in France was 0.49 and 1.51 per 1,000 women-years, respectively, during pregnancy, and 1.06 and 2.65 per 1,000 women-years during the postpartum period.
The incidence of PE and VTE increased steadily throughout the three trimesters of pregnancy, peaking in the week following delivery. An increased risk of thromboembolism persisted for at least 10 weeks after delivery.
Hypertensive Disorders of Pregnancy
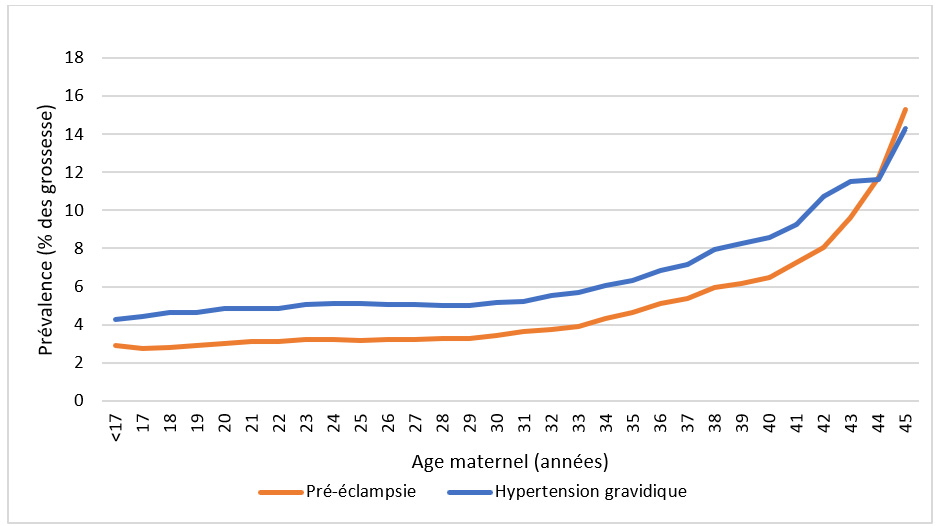
Among the 6,302,810 deliveries in the CONCEPTION cohort, the prevalence of hypertensive disorders of pregnancy was estimated at 7.4% of pregnancies (n=464,957 cases) between 2010 and 2018. Gestational hypertension and preeclampsia complicated 4.2% and 2.0% of pregnancies, respectively, during this period, averaging 29,419 and 13,923 cases per year, respectively. The prevalence of these two disorders increases with maternal age, particularly after age 40.
The prevalence of preeclampsia was higher in first pregnancies (3.1%) than in subsequent pregnancies (1.2%).
Chronic hypertension before pregnancy, which affected 1.2% of women (n=42,349), was associated with fetal complications (fetal death, low birth weight for gestational age, preterm birth) and cardiovascular complications in the mother.
Hypertensive Disorders of Pregnancy and Cardiovascular Risk
In the years following pregnancy, women who have had a hypertensive disorder of pregnancy are at increased risk for chronic hypertension, diabetes, cardio-neuro-vascular diseases, and chronic kidney disease. This risk is higher after preeclampsia than after gestational hypertension. Furthermore, when preeclampsia is early-onset, severe, recurrent, or occurs in addition to pre-existing chronic hypertension, the risk of developing cardiovascular disease is further increased.
Women who have experienced these conditions during pregnancy should therefore be informed of this risk after delivery and receive specific follow-up care. This cardiovascular risk can be significantly reduced by adopting healthy lifestyle and dietary habits, such as quitting smoking, engaging in physical activity, and eating a healthy diet.