Data
The pertussis surveillance system, Renacoq—a network for monitoring pediatric cases seen in hospitals established by Santé publique France in 1996—enables the study of epidemiological trends for this vaccine-preventable disease and the characteristics of the cases. In each of the 42 participating hospitals, the bacteriology and pediatrics departments contribute to this surveillance.
In 1996, when the network was established, cases of pertussis occurring in individuals under 17 years of age were recorded, following a diagnosis validated by clinicians and confirmed by a positive laboratory test. Since March 2016, the RENACOQ network has reported only hospitalized cases among infants under 12 months of age. A detailed clinical form is completed only for infants under 6 months of age.
Distinct epidemic cycles and very young children still the most affected by pertussis
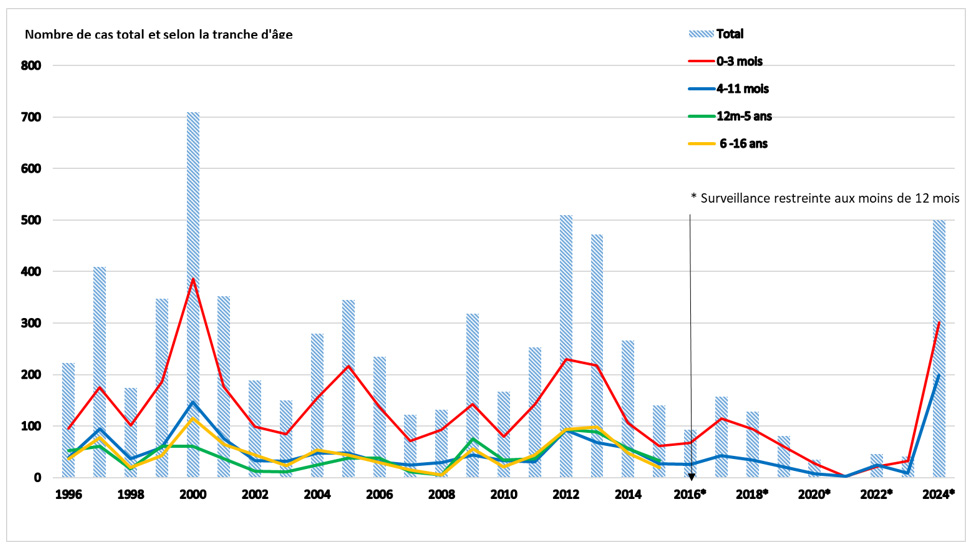
Pertussis is both a seasonal disease and one characterized by cyclical resurgences. According to data from the RENACOQ network collected from 1996 to 2024, France has experienced several epidemic cycles of varying magnitude and duration, with peaks occurring every 3 to 5 years. The regularity of these cycles was interrupted during the COVID-19 pandemic, a period during which a drastic decline in the number of cases was observed (35 cases in 2020 and 4 cases in 2021). The most recent resurgence occurred in 2024, with a total of 537 cases reported among children under 12 months of age, a level comparable to that of the year 2000 (533 cases) (Figure 1). Preliminary data for 2025 suggest a significant decline in the circulation of the bacterium within France.
Which population is most affected?
Regardless of the year, infants aged 0 to 3 months remain the age group most affected by pertussis, due to their vulnerability and the lack of full vaccine protection at this age.
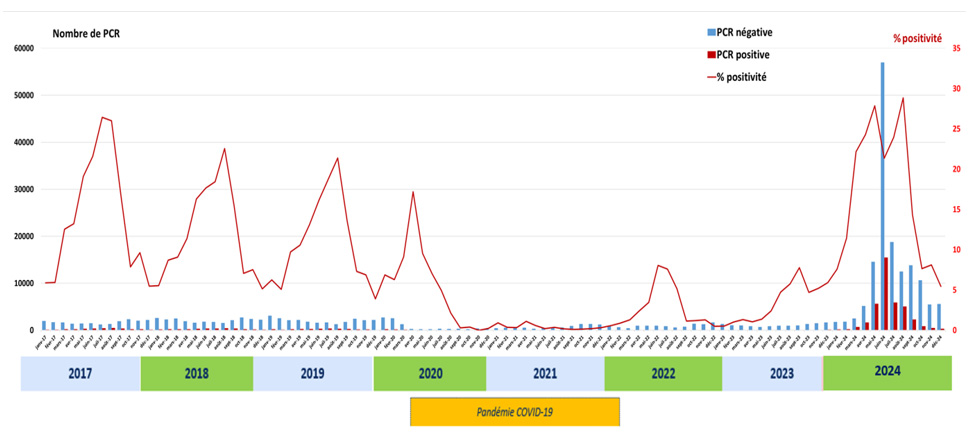
Monitoring trends in microbiological data from the 3Labos network regarding the number of PCR tests performed and the positivity rate by month and year reveals a seasonal pattern in the circulation of the bacterium, with peaks in PCR positivity observed mainly in the spring and summer; see Figure 2.
The COVID-19 period was marked by low circulation of the bacterium, followed by a gradual resurgence in 2022 and 2023 and then a resurgence in 2024.
What is the age distribution of pertussis cases?
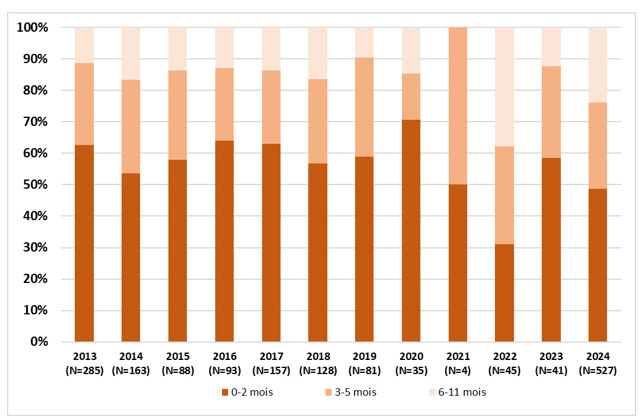
Between 2013 and 2024, among the 1,647 infants under 12 months of age hospitalized for pertussis in hospitals within the Renacoq network:
83% were under 6 months old (n=1,360)
56% were under 3 months old (n=917 infants) and therefore too young to have received the full primary vaccination series (Figure 3)
The incidence rate of cases seen in private practices skyrocketed in 2024
Between 2017 and 2024, doctors in the Sentinelles network reported a total of 829 cases of pertussis, including 689 in 2024. The estimated national incidence rates per 100,000 inhabitants showed a marked trend:
- 2017: 17 cases per 100,000 inhabitants (95% CI: 12–22);
- 2018: 10 cases (95% CI: 6–14);
- 2019: 15 cases (95% CI: 10–20);
- 2020: 3 cases (95% CI: 1–5);
- 2021: 0 cases (95% CI: 0–0);
- 2022: 0 cases (95% CI: 0–1);
- 2023: 2 cases (95% CI: 0–4);
- 2024: 244 cases (95% CI: 224–264), the highest rate since surveillance began through the Sentinelles network.
This increase marks the return of pertussis after a period of very low circulation during the COVID-19 pandemic.
Learn more about the Sentinelles network data.
Deaths are rare but can occur in very young, unvaccinated infants as well as in older individuals
More than 90% of pertussis-related deaths occur in children under 6 months of age. Between 2013 and 2024, hospitals in the RENACOQ network reported 21 deaths, 19 (90.5%) of which were in infants aged 0 to 2 months who were not yet eligible for vaccination. All of these deaths were associated with a probable source of infection within the immediate household (parents or siblings), with parents who were not up to date on their vaccinations in the majority of cases.
The year 2024 recorded 8 infant deaths, compared to only 1 in 2023. In total, analysis of data from electronic death certificates indicated 46 deaths in 2024, among them:
- 24 children were under the age of 5: 21 were under 1 year old, of whom 12 were under 2 months old;
- 22 were adults, all over the age of 50, including 15 aged 80 and older.
Annual historical data since 2015 show that 2024 is the year with the highest number of recorded deaths among children under 15 years of age.
These data underscore the critical importance of vaccinating those in close contact with infants and of maternal vaccination during pregnancy to protect newborns.
Infants remain at the highest risk of contracting severe pertussis until they are protected by vaccination, which should begin as early as 2 months of age. The primary public health challenge is therefore to prevent these infants from becoming infected through vaccination of their close contacts and through maternal vaccination (during pregnancy).
Microbiological Surveillance of Pertussis
In 2024, the National Reference Center for Pertussis and Other Bordetellosis (CNRCOQ) continued its microbiological surveillance activities in a responsive and coordinated manner with the RENACOQ network and its other partner laboratories.
The CNR received 1,430 human samples corresponding to 1,400 clinical cases, representing a 1,017% increase compared to 2023 (n=128). This sharp resurgence of B. pertussis pertussis led to increased use of culture testing, accounting for nearly 35% of the CNR’s activity. In total, 396 Bordetella isolates were characterized, including:
- 367 isolates, predominantly B. pertussis (93%),
- while B. parapertussis, B. holmesii, and other species were also identified.
Concurrently, more than 2,400 qPCR tests were performed to detect and confirm the presence of B. pertussis using specific targets and to detect the mutation conferring macrolide resistance using a PCR method developed in 2024.
Characterization of the strains in 2024 showed:
- a majority of B. pertussis expressing the vaccine antigens pertactin (PRN-positive, 96%) and FIM2 (type 2 fimbriae, 76%), in contrast to the COVID-19 period (2016–2020), when approximately 50% of strains were PRN-negative and FIM3-producing strains predominated;
- the emergence of macrolide-resistant B. pertussis (MRBP) strains, generally PRN-negative, corresponding to cases imported from Asia.
These data confirm the need for increased vigilance and an adaptable response capacity to better anticipate and manage future resurgences.
See also:
- Resurgence of Bordetella pertussis, including one macrolide-resistant isolate, France, 2024
- Microbes know no borders: importation of macrolide-resistant Bordetella pertussis into France in 2024
More information:
Vaccination coverage data
Infants: Vaccination coverage against pertussis (3 doses) at 21 months was 91.8% for children born in 2023. In this population, vaccination coverage for mandatory vaccines is generally high.
Pregnant women: vaccination coverage reached 62.3% in 2024 (compared to 43.4% in 2023), with a significant increase during 2024 (from 52% of women who gave birth in March to 75% in December 2024), though with significant regional variations. This increase could be explained by targeted communication efforts regarding vaccination conducted in the context of the 2024 epidemic and the 2022 recommendation.
Healthcare professionals: Pertussis vaccination coverage among healthcare professionals in healthcare facilities was 53.5% [95% CI: 49.9–57.0] according to a study conducted in 2019.
- Learn more about the vaccination coverage study.