Tularemia - Epidemiological Data for 2018
Note: Starting in 2018, data are reported based on the year of disease onset rather than the year of reporting, as was previously the case, in order to better reflect the epidemiology of tularemia in France. For this reason, the report will be published later in year n+1, as cases from year n are typically reported until the summer of year n+1.
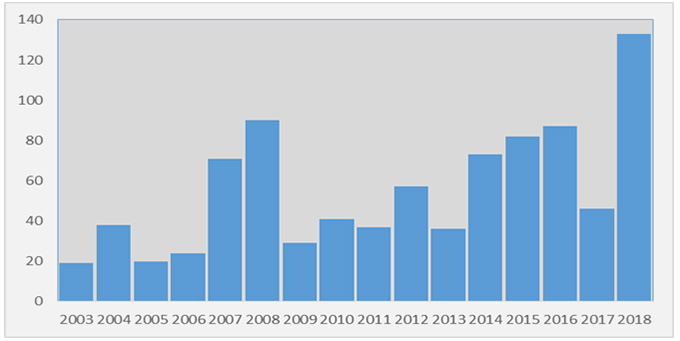
From January 1 to December 31, 2018, 133 cases of tularemia occurred in France and were reported between January 2018 and July 2019. Data from 2014 to 2016 already suggested a notable increase in the number of tularemia cases occurring and identified in France, but 2017 showed a return to a much lower number of cases, comparable to those in the years prior to 2014 (Figure 1).
In 2018, an unprecedented number of cases occurred, and the characteristics of the patients were significantly different, justifying the classification of the year as an epidemic.
Number of reported cases and spatiotemporal distribution
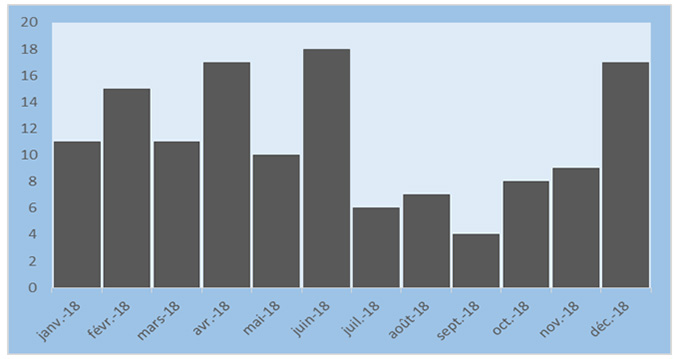
The highest number of cases was observed during the months of January through June 2018 (Figure 2).
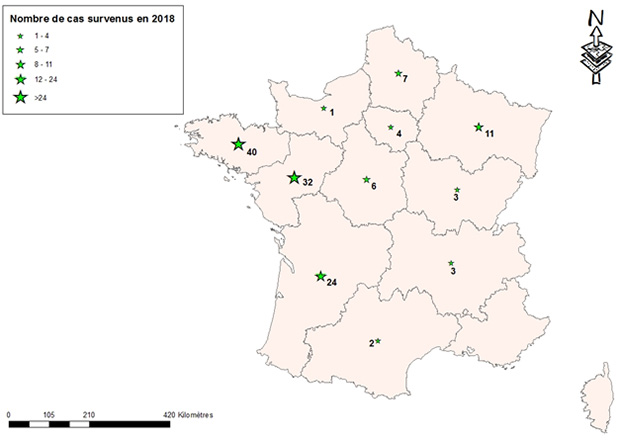
At the regional level, the hardest-hit regions were Brittany and the Pays de la Loire, which accounted for 54% of all cases. Nouvelle-Aquitaine ranked third (Figure 3).
Patient Characteristics
Of the 133 patients, 103 (78%) were male. The patients ranged in age from 3 to 91 years (median age 54 years).
Clinically, 52 (39%) patients presented with a lymph node form of tularemia, 36 (27%) with an ulcerative-lymph node form, 28 (21%) with a pleuropulmonary form, 12 (9%) with a typhoid form, and 4 (3%) with an oropharyngeal form.
Ninety-six patients (76%) had fever, and 101 (78%) had lymphadenopathy. Among patients with lymphadenopathy, the affected lymph nodes were inguinal (n=32), axillary (n=29), mediastinal (n=20), antecubital (n=15), and ENT (n=13), with 3 cases unspecified. A patient could have multiple lymph node involvement.
Fifty-one cases (40%) were hospitalized. Two patients died following pleuropulmonary tularemia.
Laboratory diagnosis
The laboratory diagnosis of the infection was established by serology alone in 85 patients, by gene amplification alone in 16 patients, by Francisella isolation alone in 14 patients, by serology and gene amplification in 10 cases, by serology and bacterial isolation in 3 cases, by bacterial isolation and gene amplification for 2 cases, and by all 3 techniques for 1 case.
The 20 isolated strains were obtained from a collection fluid aspiration (n=7), blood cultures (n=6), skin lesion swabs (n=3), lymph node biopsies (n=2), and a joint fluid aspiration (n=1). The source of the last strain was not specified.
Risk exposures
Risk exposures recorded on the DO form pertain to the 15 days preceding the onset of symptoms. Nineteen (14%) patients had handled hares, 8 (6%) rabbits, 6 (5%) a wild boar, 1 (0.7%) deer, and 23 (17%) had had intentional or accidental contact with rodents or their droppings.
Twenty (15%) patients reported a tick bite.
Twenty-eight (21%) patients reported occupational exposures likely to expose them to Francisella tularensis (14 in the agricultural sector, 6 in the gardening and landscaping sector, 3 woodworking industry workers, 1 zoologist, 1 at an agricultural high school, 1 cook who frequently prepared game, and 1 at an equestrian center).
Ninety-two (64%) cases reported outdoor recreational activities. The nature of these activities was reported for 66 cases, primarily running, trail running, or hiking (16/66), walking (15/66), hunting (15/66), gardening (11/66), mountain biking (7/66), fishing (1/66), beekeeping (1/66), and horseback riding (1/66).
For 27 (20%) cases, which were sporadic and occurred in rural areas, no risk exposure could be identified through questioning, and the source of their infection remains undetermined.
Conclusion
The year 2018 saw the highest number of identified cases since the disease was declared a notifiable disease in October 2002. This epidemic year was marked by a concentration of cases in the Pays de la Loire and Brittany regions, and a change in the characteristics of identified cases compared to previous years, with more pulmonary forms and more cases with no identifiable risk exposure.
Further surveillance will help determine whether this particular year is part of a trend or an isolated event.