Summary of Legionnaires' disease cases reported in France in 2016
Number of reported cases and incidence
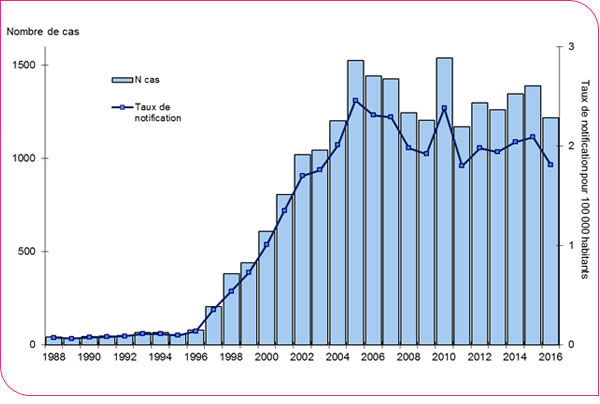
In 2016, 1,218 cases of Legionnaires’ disease were reported in France. Of these, 24 cases were residents of the French overseas departments, including 16 on Réunion Island, and 23 were foreign nationals diagnosed in France. The incidence rate of reported cases of Legionnaires’ disease in mainland France was 1.8 per 100,000 inhabitants (Figure 1). The number of cases reported in 2016 was lower than in 2015, when 1,389 cases were reported with an incidence of 2.1 per 100,000 inhabitants.
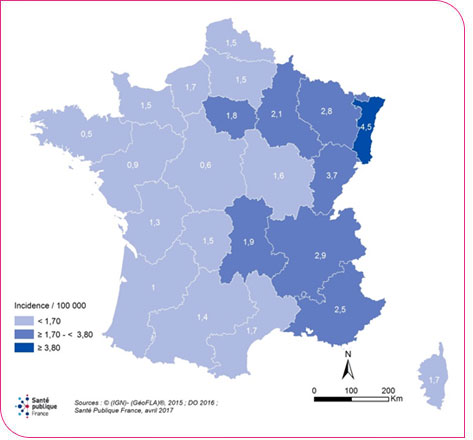
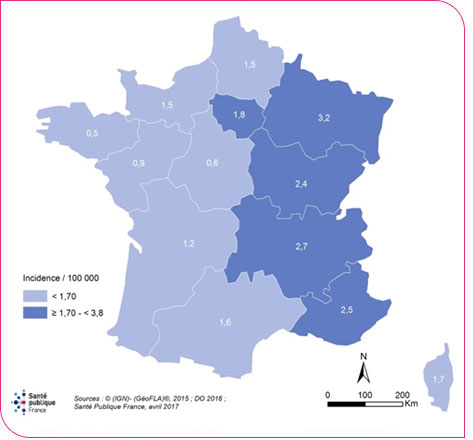
The west-to-east geographical gradient in the incidence rate of reported cases of legionellosis remained pronounced, with incidence ranging from 0.5 per 100,000 inhabitants in Brittany to 4.5 per 100,000 inhabitants in Alsace (Figure 2). The gradient was also pronounced when the new regions were taken into account (Figure 3).
Case characteristics
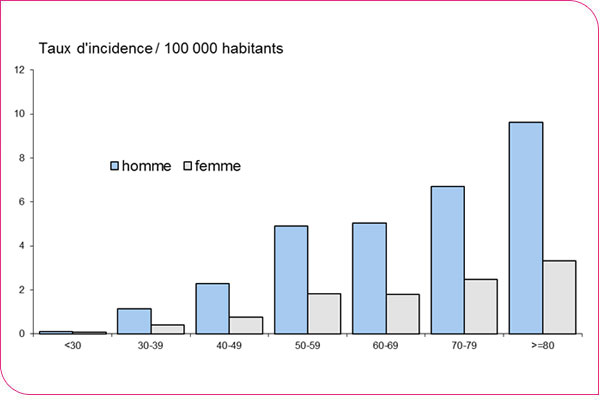
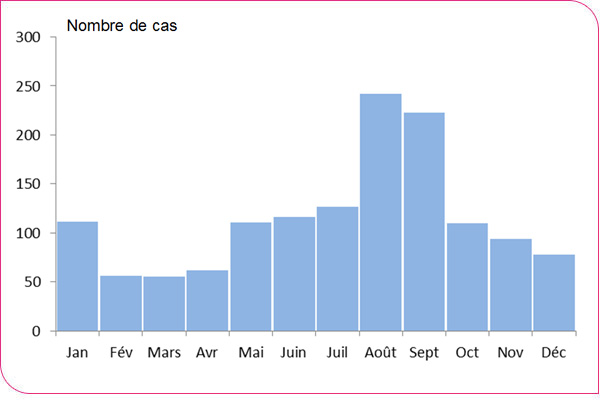
The median age of cases was 63 years [Min-Max: 17–106 years], and the male-to-female ratio was 2.3 (846 men and 372 women). Incidence increased with age, and the highest incidence rates were observed among people over 80 years of age (5.5 per 100,000) (Figure 4). Only 11 cases had not been hospitalized. The majority (76%) of cases occurred between May and October, with a peak in June, unlike in 2015, when the number of cases was high in August and September (Figure 5).
77% of cases (938 out of 1,218) had at least one known risk factor (Table 1). Smoking was the only risk factor identified in 33% of cases (11% had an additional risk factor).
|
Table 1. Frequency of risk factors for Legionnaires' disease cases in France, 2014–2016 |
||||||
|---|---|---|---|---|---|---|
|
2014 |
2015 |
2016 |
||||
|
Risk factors* |
N |
% |
N |
% |
N |
% |
|
Cancer / blood disorders |
152 |
11 |
177 |
13 |
156 |
13 |
|
Corticosteroid therapy/immunosuppressants |
118 |
9 |
163 |
12 |
136 |
11 |
|
Diabetes |
231 |
17 |
261 |
19 |
223 |
18 |
|
Smoking |
611 |
45 |
615 |
44 |
533 |
44 |
|
Others |
228 |
17 |
239 |
17 |
213 |
17 |
|
At least one factor |
997 |
74 |
1059 |
76 |
938 |
77 |
The disease course was known for 91% of cases (1,105/1,218), and the case fatality rate (131 deaths) was higher than in 2015 (11.9% versus 9%, p<0.05).
The median time between the onset of the first clinical signs and the date of notification to the Regional Health Agency (ARS) was 6 days (interquartile range [4–9]); 83% of cases were reported within 10 days of the onset of their first clinical signs and 95% within 20 days. These annual indicators have remained virtually unchanged since 2010.
Microbiological Information
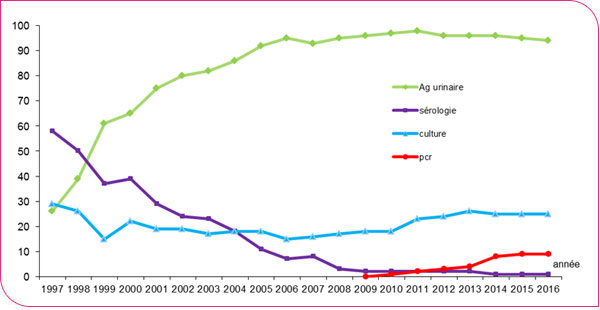
Of the 1,218 cases, 1,182 (97%) were confirmed cases, and detection of soluble urinary antigens was the primary diagnostic method used (1,149 cases, 94.3%). Polymerase chain reaction (PCR) was performed for 109 cases (9%), and for 32 of these, PCR was the sole biological diagnostic method (36 in 2015). The proportion of cases diagnosed by PCR has not increased in recent years (Figure 6). The majority of cases were associated with Legionella pneumophila serogroup 1 (Lp1) (1,168/1,218).
In 24.7% of cases (n=300), a strain was isolated; this percentage was comparable to that of 2015 (24.8%). The majority (99% = 296/300) of the strains were L. pneumophila, including 281 Lp1 and 15 belonging to other serogroups. All were analyzed using the three genotyping methods by the National Legionella Reference Center. Among the Lp1 strains, 70 (25%) were so-called “endemic” strains: 29 were “Louisa” strains, 18 were “Paris” strains, 15 were “Lorraine” strains, 6 were “Biarritz” strains, and 2 were “Mondial” strains. Among the other Lp1 strains, 174 (62%) had a profile already listed in the CNR database, and 37 (13%) had a “sporadic” profile (not yet listed). Among the 294 cases for which a sequence type (ST) was available, 39% were associated with 8 STs: ST23, ST1, ST47, ST62, ST259, ST146, ST40, and ST20; the most common were ST23 (41 cases = 14%) and ST1 (21 cases = 7%). It should be noted that, in the absence of strain isolation, complete “ST” genomic typing was performed directly on specimens for 3 cases.
For 37 cases (12%), the human-derived strain could be compared to environmental strains isolated from one or more locations frequented by the patient, and for 21 of the 39 (54%) comparisons (2 cases with 2 comparisons), the genomic profiles of the strains were found to be identical. For these cases, environmental and microbiological investigations determined that the drinking water systems were the most likely source of contamination in 8 healthcare facilities, 4 nursing homes, 6 private residences, and 3 other public facilities.
Risk exposures
Risk exposure during the incubation period (2–10 days) was reported for 460 cases (38%) (Table 2), a lower proportion than in 2015 (38% versus 42%, p<0.04). The proportion of cases that had stayed in a hospital during the incubation period in 2016 (7%) was comparable to that of 2015 (8%). Just under half of these cases (37/84) were confirmed nosocomial cases (hospitalized throughout the presumed exposure period). The 14 cases who had visited a spa were all sporadic cases. The most frequently reported mode of exposure was still the travel category (219 cases) (18% versus 22% in 2015, p=0.01). Among these cases, 151 were reported to the European Travel-related Disease Surveillance Network (ELDSNet), of which 141 cases (12% of all cases) had stayed in a hotel or campground; the other reported cases had stayed in vacation rentals, guesthouses, or accommodations booked online. Of the 151 cases, half (76 cases) had traveled abroad, and most of them to Europe (47/76 = 67%). In the “other exposures” category, 10 patients were using a continuous positive airway pressure (CPAP) device for sleep apnea (19 cases in 2015).
|
Table 2. Risk exposures among cases of Legionnaires’ disease in France, 2014–2016 |
||||||
|---|---|---|---|---|---|---|
|
Exposures* |
2014 |
2015 |
2016 |
|||
|
|
n |
% |
n |
% |
n |
% |
|
Hospital |
72 |
5 |
108 |
8 |
84 |
7 |
|
Retirement home |
63 |
5 |
55 |
4 |
54 |
4 |
|
Spa |
3 |
0 |
6 |
0 |
14 |
1 |
|
Travel |
259 |
19 |
304 |
22 |
219 |
18 |
|
Hotel-campground |
161 |
12 |
177 |
13 |
141 |
12 |
|
Temporary residence |
45 |
3 |
84 |
6 |
36 |
3 |
|
Other types of travel* |
53 |
4 |
43 |
3 |
42 |
3 |
|
Others |
103 |
8 |
108 |
8 |
89 |
7 |
|
Total cases with at |
500 |
37 |
581 |
42 |
460 |
38 |
In 2016, the European travel-associated disease surveillance network (ELDSNet) reported 29 additional cases to Santé publique France, in addition to those previously reported (59 in 2015). These cases occurred among foreign nationals who had stayed at a tourist facility in France within 10 days prior to the onset of symptoms and were diagnosed in a foreign country.
In total, based on notifications of French and foreign cases, 156 French establishments were reported by ELDSNet (264 in 2015), 145 for isolated cases and 11 for cluster cases (defined by ELDSNet as at least two cases having stayed in the same establishment over a two-year period). In these 11 facilities, an investigation involving water samples from the potable water system revealed the presence of Legionella above the regulatory threshold in 4 (36%) of them.
In 2016, several investigations of clustered cases—both temporally and spatially—were conducted by the ARS in collaboration with the Cires. Three investigations, all involving community-acquired cases, were reported to national authorities. Only one investigation involved more than 10 cases and reported an excess of cases on the island of Réunion, where 20 cases had been reported in 6 months (versus 2 to 8 cases per year). No common source of contamination could be identified during these three investigations.
Conclusion
In 2016, the number of Legionnaires’ disease cases was lower than in 2015 but has remained relatively stable since 2005, ranging between 1,200 and 1,500 cases. The incidence rate of reported cases in mainland France, at 1.8 per 100,000 inhabitants, remains higher than the European rate (1.4 per 100,000 inhabitants in 2015) but lower than that of neighboring countries (Italy and Spain) [2]. The “west-to-east” geographic gradient in the incidence rate of reported cases observed in recent years is the subject of a multifactorial study examining meteorological factors. The results of this study, which aims to explain these disparities in Legionnaires’ disease incidence across the country, will be available shortly. The overall characteristics of Legionnaires’ disease cases remain stable, and the majority of cases present known risk factors, whether related to age or a predisposing factor. As in 2015, no cases in children under 15 years of age were recorded at the national level. The proportion of reported risk exposures is lower than in 2015 but comparable to previous years, particularly regarding travel. The number of cases involving visits to a spa facility has more than doubled compared to 2015, but all cases were isolated incidents. Cases linked to the use of continuous positive airway pressure (CPAP) devices for sleep apnea are fewer than in 2015, but vigilance regarding the use of these devices in accordance with ANSM recommendations [3] must continue, with systematic investigation of every case involving this situation.
The low number of clustered cases reported at the national level demonstrates that the responsiveness of partners involved in surveillance and the appropriate management of these episodes at the regional level help limit their scope. The high number of cases on Réunion Island has helped clarify the diagnostic methods used and strengthen collaboration among the various partners involved in regional surveillance. However, the majority of investigations have not identified the sources of contamination. Documenting known or new sources of contamination remains a priority. It is essential to maintain the responsiveness of local partners and to thoroughly investigate all clusters of cases, as well as to continue promoting clinical specimen collection, which provides access to strains and thus enhances the ability to identify sources of contamination and document clusters of cases.
[2] European Centre for Disease Prevention and Control. Annual epidemiological report for 2015 – Legionnaires’ disease. [Internet]. Stockholm: ECDC; 2017.
[3] ANSM Recommendations, 2016: http://ansm.sante.fr/S-informer/Points-d-information-Points-d-information/Dispositifs-medicaux-d-assistance-respiratoire-utilises-a-domicile-Recommandations-destinees-aux-patients-Point-d-Information