The disease
Hepatitis E, a zoonotic disease in France
Hepatitis E is an infection caused by a virus that leads to liver damage (hepatitis). There are several genotypes of the hepatitis E virus (HEV). Genotypes 1 through 4 are responsible for the majority of infections in humans. Genotypes 1 and 2 circulate primarily in developing countries, where the disease is endemic and epidemic, and is transmitted via the fecal-oral route and through the consumption of contaminated water. This situation is caused and exacerbated by challenges related to sanitation and the supply of drinking water.
The situation is different in industrialized countries such as France, where hepatitis E is also endemic but is primarily linked to genotype 3 and, to a lesser extent, genotype 4. The main mode of transmission for genotype 3 HEV is the consumption of contaminated products from HEV reservoir animals in Europe, particularly pigs. However, environmental contamination (particularly of water) also appears to play a role. Hepatitis E is a zoonosis, transmitted from animals to humans in France.
HEV infection is asymptomatic in the majority of cases. When it causes symptoms, these are primarily those of acute viral hepatitis, not unlike those of hepatitis A, with general signs such as fever, fatigue, and abdominal pain, followed by jaundice (yellowing of the skin and mucous membranes). Extrahepatic symptoms are not uncommon, including neurological, renal, or hematological complications. People with chronic liver disease are at risk for more severe forms of hepatitis E (fulminant hepatitis, death). Furthermore, unlike hepatitis A, HEV genotype 3 can also cause chronic hepatitis with rapid progression to cirrhosis in immunocompromised individuals.
It should be noted that HEV genotype 1, which circulates in developing countries, can cause fulminant hepatitis and death, particularly in pregnant women.
Although hepatitis E is less widely recognized than other viral hepatitis types as a cause of acute hepatitis in France, it is nevertheless one of the most common forms there. Santé publique France participates in monitoring the epidemiological trends of hepatitis E in collaboration with the National Reference Center (CNR) for enterically transmitted hepatitis viruses. Santé publique France also provides information to healthcare professionals to raise their awareness of the disease and enable appropriate control measures whenever possible.
The infectious agent
The hepatitis E virus, first identified in 1983, belongs to the Hepeviridae family, genus Hepevirus. It exhibits significant genetic diversity, with four major genotypes, each further divided into several subtypes.
Genotypes 1 and 2 are endemic in developing countries, and humans are the sole reservoir in these countries.
Genotype 3 is endemic in European Union countries. Viruses of genotypes 3f, 3c, and 3e are the most common there.
Genotype 4 is found primarily in Asia (China, Japan) but has also been identified, albeit rarely, in humans and pigs in Europe.
Genotypes 3 and 4 are found in humans and in numerous animal species such as chickens, rats, rabbits, ferrets, rainbow trout, and bats; however, the primary animal reservoir for HEV in France is the pig and, more generally, suids (domestic pigs, wild boars).
Like all non-enveloped enteric viruses, HEV is relatively resistant in the external environment, and viral particles can be detected in wastewater. In vitro, it is sensitive to heat (autoclaving at 120°C) and to disinfectants commonly used to inactivate enteric viruses (sodium hypochlorite for water treatment, glutaraldehyde for surface disinfection). The presence of organic matter significantly reduces the effectiveness of these disinfectants.
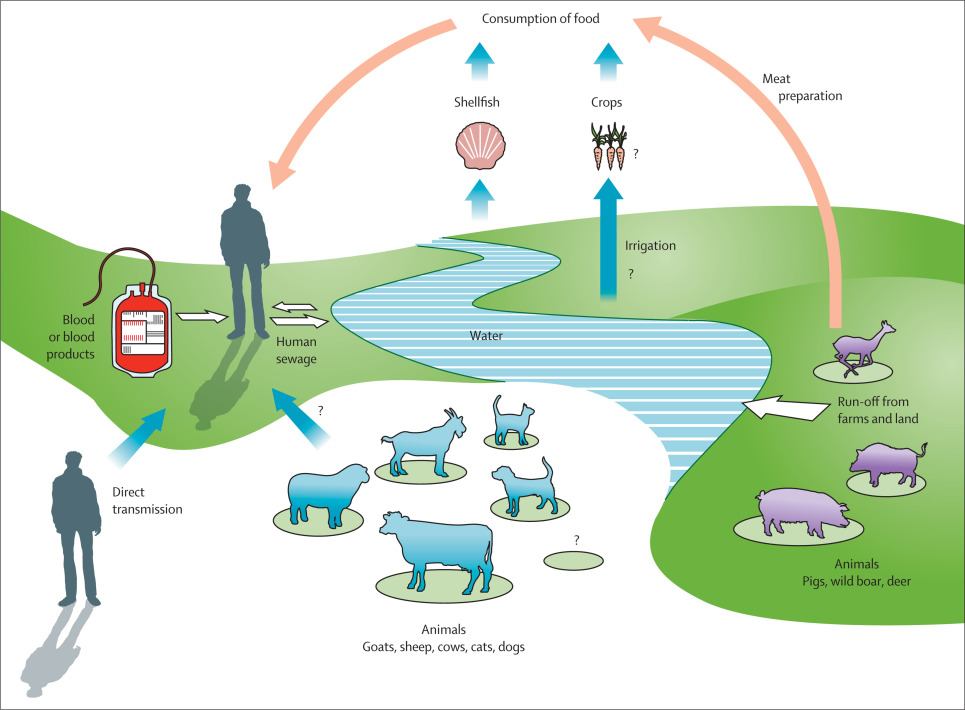
The various modes of transmission of hepatitis E
The predominant modes of transmission differ depending on the reservoir of the circulating virus.
The main documented or suspected routes of transmission of HEV genotype 3 to humans in France are:
consumption of meat from an infected animal, particularly raw or undercooked pork liver;
consumption of water or unpeeled, raw fruits or vegetables contaminated with human or animal feces;
consumption of seafood farmed in contaminated waters;
more rarely, transfusion of blood products or organ transplantation from individuals infected with HEV.
The list of implicated foods includes wild boar and deer meat and offal, particularly offal (heart, spleen, liver, lungs), pork liver (fresh, dried), and products made from raw pork liver (liver sausage, figatelli, fitone, dried liver sausage).
Transmission via direct or indirect contact with reservoir animals is suspected in certain populations, such as hunters, people working in occupations involving contact with wildlife or pigs, and veterinarians in industrialized countries.
In developing countries where genotypes 1 and 2 of the virus circulate, the reservoir is exclusively human, and transmission is fecal-oral. Since drinking water supply and sanitation are not adequately managed in these areas, HEV is primarily transmitted through water. It is responsible for major epidemics. The role of certain factors, such as the method of storing drinking water and washing hands in the same container as infected individuals, has been suspected. Person-to-person transmission has also been considered during these waterborne outbreaks.
Mother-to-child transmission has been well documented in developing countries. Very rare cases have been reported in industrialized countries.
Laboratory Diagnosis
The diagnosis of hepatitis E relies on the detection of specific IgM and IgG antibodies and on the detection of the viral genome in blood or stool. The CNR, as part of its virological expertise, is responsible for characterizing strains (viral genotypes and subtypes).
The progression of biological markers during HEV infection (RNA in blood or stool, anti-HEV IgM and IgG) is summarized and available on the CNR website.
Acute hepatitis E is defined by the presence of anti-HEV IgM in the blood or by the presence of the virus in the blood or stool. For clinicians, the CNR provides a diagnostic algorithm tailored to different situations (immunocompetent or immunocompromised patients). The presence of isolated anti-HEV IgG indicates prior exposure to HEV.
Prevention of Hepatitis E
In France, the prevention of locally acquired cases of hepatitis E relies on general personal hygiene measures and precautions taken during food preparation or consumption:
washing hands after using the restroom, before preparing meals, and after contact with animals or animal products;
cleaning utensils and surfaces after handling products made from raw pork liver, wild boar meat, or venison;
cooking food intended for consumption thoroughly;
following the cooking and consumption instructions on product labels;
do not drink untreated water (from wells, springs, streams, etc.).
It is particularly recommended to cook high-risk products thoroughly:
products made from raw pork liver (fresh or dried liver sausages, figatelli);
made from wild boar or deer (meat and offal), particularly offal (heart, liver, spleen, lungs).
A labeling system for products made with raw pork liver was implemented in 2009, recommending that these products be cooked thoroughly.
Consumption of these products, even when cooked, is not recommended for people at risk of developing a severe form of hepatitis E (immunocompromised patients, patients with pre-existing chronic liver disease, and pregnant women) (learn more: http://www.sante.gouv.fr/IMG/pdf/Fiche_Hepatite_E.pdf).
In two opinions, ANSES assessed the impact of processing methods (heat treatment, drying) on the survival of HEV in products made from raw pork liver, such as products cooked by a professional (Alsatian liver sausages or Alsatian liver salami, liver mousses (pâté) and Alsatian liver quenelles), products cooked by the consumer (fresh liver sausages from the Southwest), and products consumed raw (figatelli, dried liver sausages, dried salted liver). Heat treatment to a core temperature of 71°C for 5 minutes is recommended for the decontamination of pork liver mixtures, and for 20 minutes for complex matrices such as those found in figatelli. Drying as practiced by manufacturers of raw liver-based products cannot be considered effective for inactivating HEV.
In developing countries, the primary prevention of hepatitis E consists of improving sanitation infrastructure and access to safe drinking water. Prevention of hepatitis E for travelers to HEV-endemic areas relies on traveler advisories regarding enteric risks.
Download

Although no hepatitis E vaccine is currently available in France, two vaccines have been tested in Nepal (the rHEV vaccine) and in China (the HEV239 vaccine), with one showing 95.5% efficacy and the other between 94% and 100% efficacy in preventing symptomatic forms of hepatitis E. The use of the HEV239 vaccine has been approved only by China at this time.
Clinical presentation and prognostic factors
Hepatitis E is asymptomatic in 65% to 95% of cases, depending on the study. However, after an incubation period of 2 to 8 weeks (40 days on average), infection with the hepatitis E virus can lead to symptoms of acute hepatitis similar to those of hepatitis A: fever, fatigue, nausea, vomiting, loss of appetite, and abdominal pain, often followed by jaundice (68%–86%).
Hepatitis E can also cause extrahepatic symptoms, particularly central or peripheral neurological symptoms (Guillain-Barré syndrome, Parsonage-Turner syndrome, polyradiculitis, encephalitis, etc.), as well as renal or hematological symptoms.
Hepatitis E most often resolves spontaneously within 3 to 5 weeks. However, in rare cases, it can progress to a fulminant form that may require a liver transplant and lead to death. These severe forms of hepatitis E are primarily observed in individuals with pre-existing chronic liver disease.
Genotype 1 of the virus causes severe forms in pregnant women, with death occurring in 15 to 20% of cases, particularly during the third trimester of pregnancy. Therefore, in France, when hepatitis E is diagnosed in a pregnant woman, it is advisable to inquire about travel to areas where genotype 1 is endemic to assess the prognosis of the infection.
Genotype 3 of the virus, on the other hand, can cause chronic forms of hepatitis E in immunocompromised individuals due to organ transplantation, malignant hematological disease, or other acquired immunodeficiencies (HIV infection, etc.).
Management and Treatment of Hepatitis E
Immunocompromised individuals and those with pre-existing chronic liver disease must be closely monitored by a physician due to the risk of complications (fulminant hepatitis, progression to a chronic form of hepatitis E, cirrhosis).
Most patients recover spontaneously and do not require specific treatment. In cases of severe hepatitis, treatment focuses on symptomatic management and may extend to liver transplantation in cases of fulminant hepatitis.
Chronic hepatitis caused by acquired immunodeficiency can be cured if the underlying immunodeficiency can be resolved. Treatment with ribavirin has also proven effective in certain cases of chronic hepatitis, leading to a cure with a sustained virological response. Ribavirin treatment may also be recommended in cases of severe extrahepatic manifestations.