The disease
An infectious disease
Dengue is an infectious disease caused by an arbovirus: the dengue virus. This virus is transmitted by mosquitoes of the genus Aedes: Aedes aegypti and Aedes albopictus (the latter is also known as the tiger mosquito).
It belongs to the Flaviridae family (genus Flavivirus) and has four different serotypes (DEN1 to DEN4).
Infection with one serotype induces immunity against that serotype but not against the others, so it is possible to be infected multiple times by different dengue serotypes. While the disease is asymptomatic in most cases, the typical form presents with sudden fever accompanied by body aches and a rash. In rare cases, serious and sometimes fatal complications may occur.
In this context, Santé publique France’s priorities are:
Defining, managing, and coordinating the epidemiological surveillance of dengue in France
Adapting surveillance to regional specificities and risks: enhanced surveillance systems in metropolitan departments where the mosquito vector is present, and specific systems for the various overseas departments in collaboration with regional intervention units linked to regional health agencies
Contributing to the information and awareness of healthcare professionals, local authorities, and the general public regarding the disease and preventive measures.
Several modes of dengue transmission
Vector-borne transmission
The dengue virus is primarily transmitted by mosquito vectors. Dengue vectors are mosquitoes of the genus Aedes, primarily Aedes aegypti and Aedes albopictus (the tiger mosquito).
Dengue is an infection that is most prevalent in tropical and subtropical regions where the vectors Aedes aegypti and Aedes albopictus are present. Aedes albopictus is also present in temperate zones, particularly in Europe, including mainland France, where a few transmission events have been identified.
In France, Aedes aegypti is found in the French West Indies, French Guiana, and Mayotte, while Aedes albopictus is found on Réunion Island and in several mainland departments.
These Aedes mosquitoes develop primarily in urban areas and do not move far during their lifetime. Females lay their eggs in breeding sites where stagnant water is necessary for larval development: pots, saucers, used tires, poorly drained gutters, various types of waste containing stagnant water, as well as tree hollows and certain plants that can retain water (bamboo, etc.). Man-made breeding sites are the primary locations where these mosquitoes lay their eggs.
Aedes bites occur mainly during the day, with peak activity at dawn and dusk. When biting an infected person in the viremic phase, the mosquito picks up the virus from that person’s blood. The virus then multiplies within the mosquito for approximately 10 days, known as the extrinsic phase. At the end of this extrinsic phase, the mosquito can transmit the virus and infect a new person during another bite.
For dengue, the viremic phase begins approximately 1 to 2 days before the onset of clinical symptoms and lasts up to 7 days afterward.
In 2018, Aedes albopictus (also known as the tiger mosquito) was established and active in 51 departments (out of the 96 metropolitan departments).
Aedes albopictus (also known as the tiger mosquito) is primarily an urban, anthropophilic species. The departments in which the tiger mosquito is established and active—that is, where it is permanently established and breeding—are classified as Level 1 under the national plan to prevent the spread of chikungunya, dengue, and Zika.
Transmission via human-derived products
The virus can, more rarely, be transmitted through transfusion or transplantation (of organs or cells).
Symptoms and complications
Dengue is asymptomatic in 50 to 90% of cases (percentage varies depending on the outbreak).
For the 50 to 10% of infected individuals who develop symptoms, the incubation period lasts an average of 4 to 7 days (but can range from 3 to 14 days)
The “classic” form presents with a high fever that begins suddenly. It is often accompanied by chills, headache, retro-orbital pain, nausea, vomiting, joint and muscle pain, and, inconsistently, a rash around the 5th day of symptoms. The course is usually favorable after a few days
The severe form (or severe dengue) can occur in 1% to 5% of symptomatic cases (WHO 2009). It is characterized by increased vascular permeability, which can lead to shock and life-threatening hemorrhages.
Warning signs appear 2 to 7 days after the onset of symptoms and following a return to normal body temperature (resolution of fever),
Clinical vigilance must be at its highest around the 4th day.
Treatment for dengue is symptomatic. There is no specific antiviral treatment.
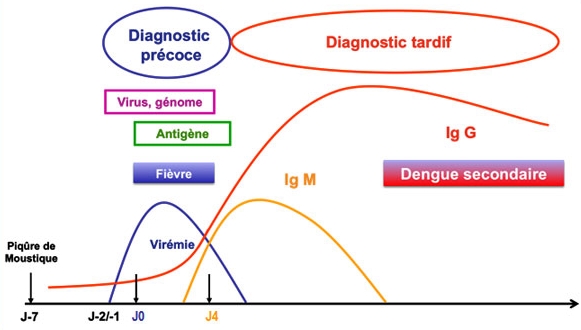
Primary dengue and secondary dengue
There are 4 serotypes of the dengue virus. Infection with one serotype confers immunity against that serotype but not against the others.
We refer to:
Primary dengue during a first infection with the dengue virus
Secondary dengue when an individual is reinfected by another serotype The risk of developing a severe form appears to be higher in secondary dengue than in primary dengue.
Diagnosis
The diagnosis of dengue virus infection is made using techniques that allow for:
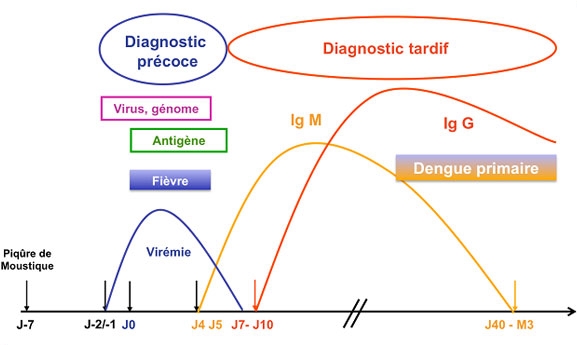
Detect the viral genome, viral antigens, or the virus: gene amplification (RT-PCR), detection of the NS1 antigen, viral culture. The NS1 antigen, of limited value in geographic areas where the disease incidence is low, is not recommended in mainland France.
Detect antibodies: this is serology
IgM antibodies appear starting on the fifth day after the onset of clinical symptoms and persist for an average of 2 to 3 months
IgG antibodies appear shortly after (primary dengue) or at the same time (secondary dengue) as IgM antibodies and persist for life.
In the presence of IgG alone (without IgM), a diagnosis of dengue can only be established if there is an increase in antibody titer (IgG) in successive samples taken at a minimum interval of 10 days, indicating a recent infection. Early testing (up to Day 7) by RT-PCR should be prioritized due to its significantly higher specificity compared to serology
It is essential to accurately identify the date of symptom onset (DSO) to guide further testing.
The diagnostic protocol recommended in the Ministry’s “Plan to Prevent the Spread of Chikungunya and Dengue” is as follows:
Up to 5 days after the onset of symptoms (D5): RT-PCR
Between D5 and D7: RT-PCR and serology
After D7: serology only (IgG and IgM) with a second confirmatory sample taken no earlier than 10 days after the first sample
Blood samples can be collected by any clinical laboratory.
Each sample must be accompanied by a clinical information form.
Preventing Dengue
Dengue prevention relies on individual and collective actions
Individual prevention:
There is a vaccine against dengue (Dengvaxia®). The HAS issued two unfavorable opinions in 2018 and 2019 regarding the use of the Dengvaxia® vaccine in the strategy to combat dengue in France’s overseas departments. Indeed, the marketing authorization is restrictive, as this vaccine is indicated only for individuals aged 9 to 45 living in endemic areas and further requires a pre-vaccination serological test to exclude individuals who are seronegative for dengue from vaccination. In fact, for these individuals, the vaccine poses a risk of severe dengue in the event of subsequent infection. However, there is currently no screening test for a history of dengue virus infection of sufficient quality to implement such screening at the population level. Nevertheless, the HAS considers that vaccination with Dengvaxia® may be offered to individuals living in French territories in the Americas who provide documented proof of a previous, virologically confirmed dengue virus infection. Furthermore, this vaccine is not intended for travelers.
Individual prevention therefore relies primarily on measures to protect against mosquito bites: repellents in sprays or creams, coils, electric diffusers, long clothing, and mosquito nets.
Protection is particularly necessary during the day, as Aedes mosquitoes—the primary vectors—bite mainly during daylight hours, primarily outdoors, with peak activity in the early morning and late afternoon.
LEARN MORE

magazines/revues
8 June 2022
Weekly Epidemiological Bulletin, June 2, 2022, Special Issue: Health Recommendations for Travelers, 2022 (for healthcare professionals)
Community-based prevention and vector control
Collective mosquito prevention and control also rely on vector control and community-based control.
The control of disease-carrying vectors, such as mosquitoes, is referred to as vector control. In its broadest sense, vector control encompasses both the control of and protection against these insects. Vector control relies on methods that vary depending on the vector and the epidemiological and socioeconomic contexts. It includes chemical control, biological control, genetic control, environmental interventions, health education, community mobilization, and the ongoing evaluation of all these methods.
Its objective is to contribute, alongside other public health initiatives, to reducing the risks of endemicity (the long-term establishment of a disease in a region) or epidemic outbreaks, to reducing the transmission of pathogens by vectors, and to managing outbreaks of vector-borne diseases, all within a formalized strategic framework.
Depending on the scale at which this mosquito control is carried out, a distinction is made between control at the regional level (departments, municipalities) and that carried out at the individual level, which specifically targets mosquito breeding sites located in the immediate vicinity of homes.
Vector control at the regional level is carried out by public mosquito control agencies. Chemical control has two components:
Larvicides, which specifically target mosquito larvae
Adulticides, which specifically target adult mosquitoes
Community-based control, which is everyone’s responsibility, relies on:
The elimination of potential larval breeding sites around homes (standing water in saucers, gutters, vases, buckets, trash, etc.)
Personal protection against mosquito bites
A mosquito established in mainland France
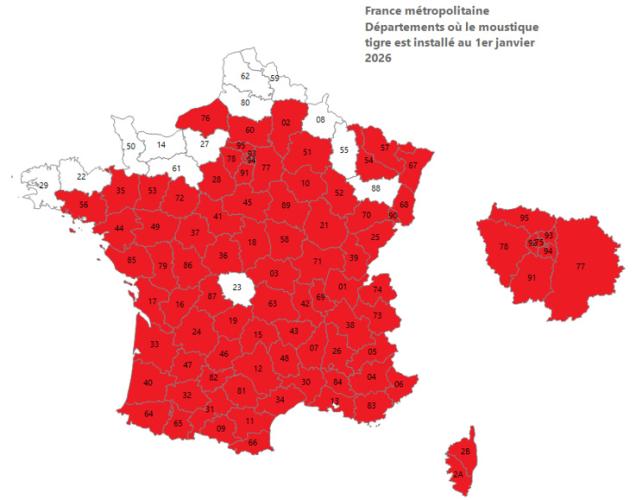
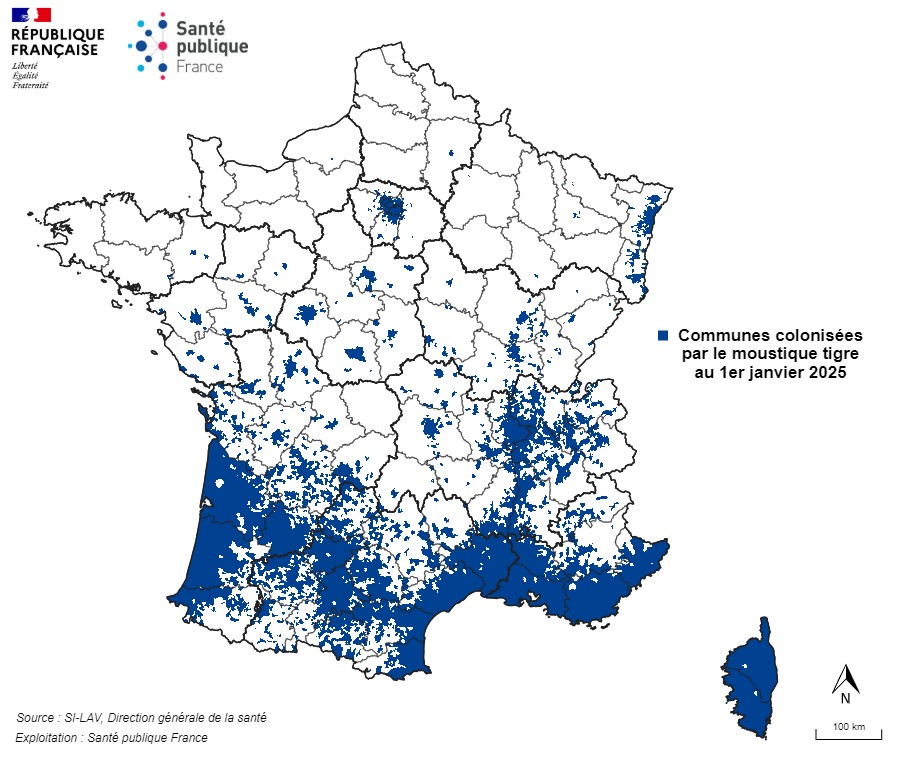
Aedes albopictus (also known as the tiger mosquito) is considered the most invasive mosquito species in the world. It is native to Southeast Asia, from where it spread from east to west via commercial transport. In Europe, it was first identified in Albania in 1979 and then in Italy starting in 1990. It has been established in southern France since 2004 and has been gradually spreading since then.
By early 2024, 78 departments were colonized by the Aedes albopictus mosquito (out of the 96 metropolitan departments).