Evaluation of the Colorectal Cancer Screening Program for the 2016–2017 Period: National Indicators
Reminder: The guaiac test (Hemoccult® II) was replaced by the immunological test (OC Sensor®) in April 2015. This subsection presents follow-up data for individuals who participated in the program between January 1, 2016, and December 31, 2017.
A description of the indicators is available in the Data Format Guide and Definitions of Indicators for the National Program Evaluation.
Indicators of Screening Test and Diagnostic Test Quality
The national quality indicators for screening tests and diagnostic examinations are listed in the table (xlsx format and pdf format).
Test Performance Quality
A total of 5.6 million people underwent a screening test between January 1, 2016, and December 31, 2017. Of these, 406,000 (7.2%) had a test that proved unanalyzable. The proportion of people with an unanalyzable test was similar among men and women. It was higher for a first screening (8.7%) than for a subsequent screening (6.6%).
The main reasons for unanalyzable tests were: expired tube (42.4%), missing collection date (35.7%), and sample collected more than 6 days prior (10.4%).
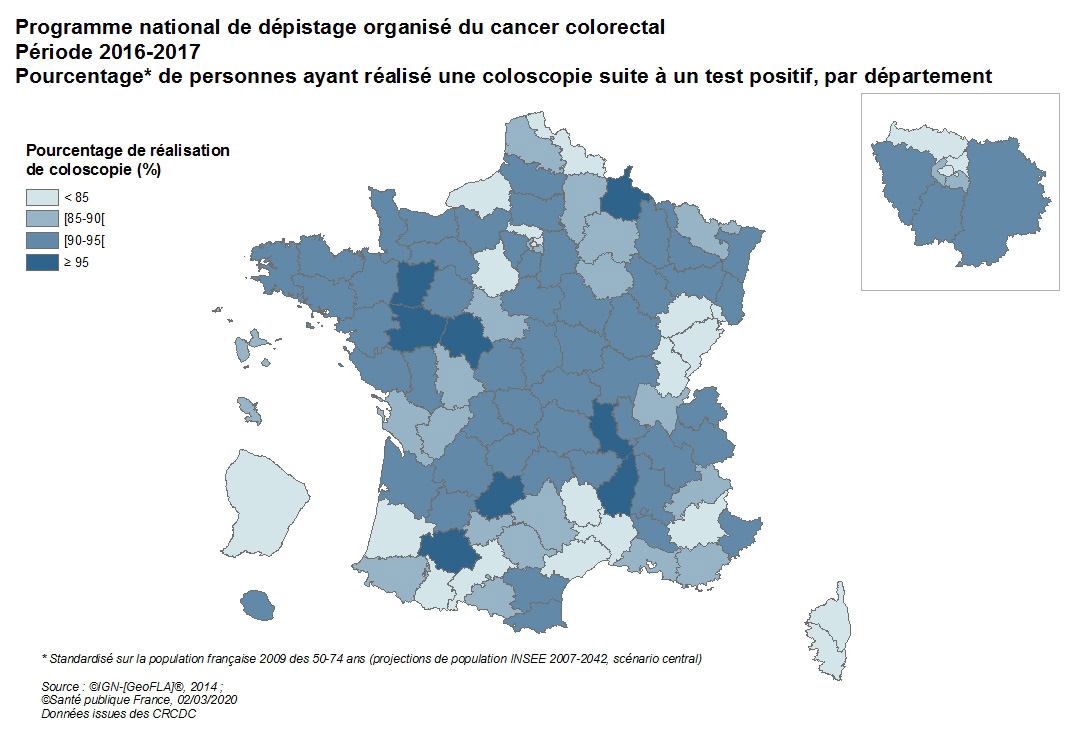
Percentage of people who underwent a colonoscopy following a positive test
Of the 247,989 people eligible for a colonoscopy after a positive test, 217,795 underwent a colonoscopy (88.9%). This figure is close to the recommended European benchmark (90%). This colonoscopy completion rate, which remained stable compared to the 2013–2014 period (88.6%), varied by department. Nineteen departments had rates below the acceptable European benchmark (85%).
Quality of Colonoscopy Preparation
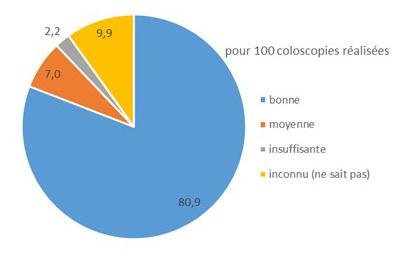
The quality of preparation for colonoscopies was rated as good for 80.9% of exams, average for 7.0%, and inadequate for 2.2%. Information on the quality of the colonoscopy was missing for 9.9% of exams.
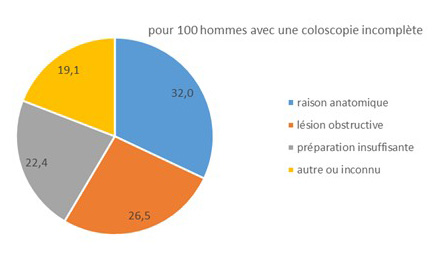
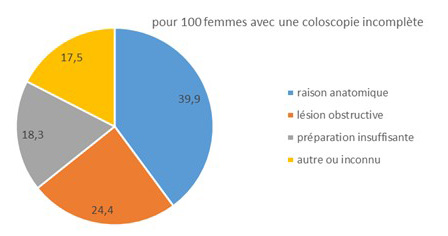
A colonoscopy is considered incomplete if the entire colon and rectum are not examined during the procedure. The percentage of people who underwent a complete colonoscopy was 92.7% (men: 92.9%; women: 92.5%). This figure is slightly higher than the acceptable benchmark recommended at the European level (90%) and lower than the desirable benchmark (95%). This figure remained stable compared to the 2013–2014 period (93.4%). The reasons why colonoscopies were incomplete varied by sex: 32.0% of cases due to anatomical reasons among men versus 39.9% among women; 26.5% among men due to obstructive lesions versus 24.4% among women; and 22.4% due to inadequate preparation among men versus 18.3% among women.
Follow-up on examinations
Colonoscopy Morbidity
The completeness of data collection on colonoscopy complications, particularly deaths occurring in the days following the procedure, cannot be guaranteed at the national level. In fact, for 49.6% of colonoscopies, the variable recording colonoscopy incidents and accidents was not filled in, making it impossible to determine whether the information is missing or whether the colonoscopy proceeded without complications. Nevertheless, at the national level, 807 colonoscopy incidents and accidents were recorded, including 118 perforations. Given the incompleteness of these data, the statistics on colonoscopy morbidity cannot be used as is.
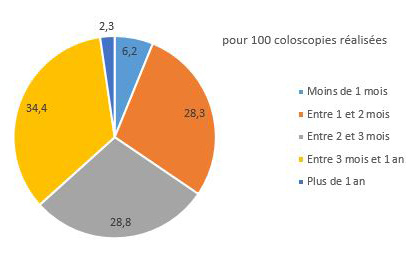
Timeframes for performing colonoscopies
The distribution of wait times for colonoscopies following a positive test shows that only 6.2% of colonoscopies are performed within one month, in accordance with European benchmarks. The median wait time is 76 days (vs. 62 days in 2013–2014). It varies by department: the shortest median wait times (less than 2 months) are observed in the departments of Alpes-Maritimes, Lozère, and Morbihan, and the longest (over 3.5 months) in the departments of Haute-Saône and Territoire-de-Belfort.
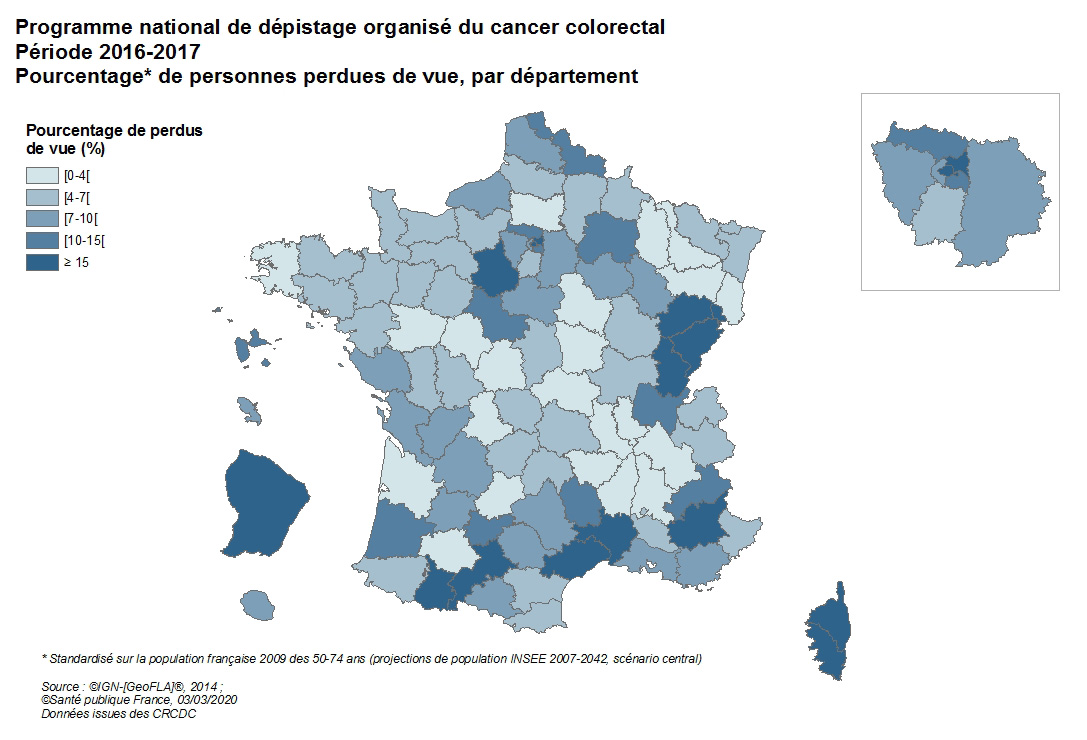
Lost to follow-up
A person is considered lost to follow-up when the CRCDC is unable to obtain any information about that person 24 months after the positive test result. The percentage of people lost to follow-up is 7.3% (7.6% among men and 7.0% among women) for all departments participating in the program. This percentage varies by department: from less than 2% in the departments of Allier, Isère, Loire, Rhône, Yonne, Vosges, Gironde, and Gers to more than 20% in the departments of Jura, French Guiana, and Hautes-Pyrénées. These departmental disparities reflect the heterogeneity in the quality of data collection regarding the follow-up of individuals who tested positive (for example, the transmission of information on the tests performed and their results by healthcare professionals to the CRCDC is more or less systematic). Individuals who tested positive, with whom direct or indirect contact was possible, and who were informed of the positive result but did not undergo a colonoscopy will be considered ineligible for screening after two years and following a final reminder letter.
Lesions detected
These are indicators relating to the nature and rates of lesions detected (adenomas, advanced adenomas, and cancers) through diagnostic examinations (colonoscopy or other). These indicators are listed in the table (xlsx format and pdf format).
Over the 2016–2017 period, the program detected 67,899 advanced adenomas and 17,061 colorectal cancers.
The detection rate for advanced adenomas (and colorectal cancers, respectively) is defined as the proportion of patients in whom an advanced adenoma (or cancer, respectively) is the most serious lesion detected, among those who underwent an analyzable screening test. It is expressed per 1,000 (‰) screened individuals.
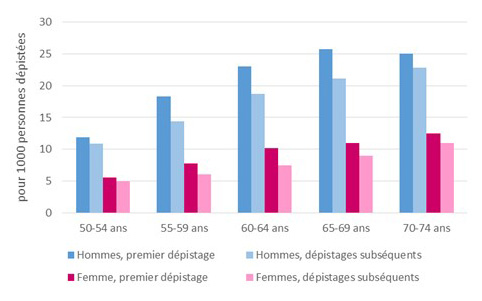
The detection rate for advanced adenomas (adenomas 10 mm or larger, or with high-grade dysplasia, or a villous component) was 12.3 per 1,000 screened individuals.
The detection rate for advanced adenomas was higher among men (17.7‰) than among women (7.8‰); it increased with age, rising from 11.6‰ among men aged 50–54 to 23.1‰ among those aged 70–74, and from 5.4‰ among the youngest women to 11.2‰ among the oldest. It was also, for both men and women, higher during the first screening than during subsequent screenings, regardless of age group (see figures below).
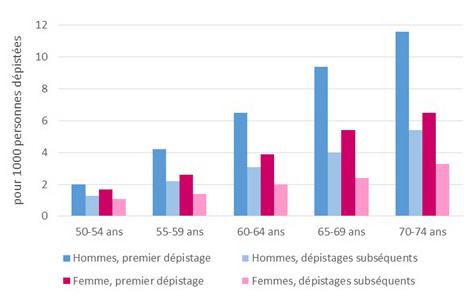
The cancer detection rate was 3.0 per 1,000 people screened.
The cancer detection rate was higher among men (4.1‰) than among women (2.1‰); it increased with age, rising from 1.9‰ among men aged 50–54 to 7.2‰ among those aged 70–74, and from 1.2‰ among younger women to 7.6‰ among older women. It was also, for both men and women, higher during the first screening than during subsequent screenings, regardless of age group (see figures below).
Detection rates for advanced adenomas and colorectal cancers also vary by department; they depend heavily on the incidence and prevalence of cancer in each department and on the effectiveness of departmental programs in detecting these lesions. The departmental percentages of colonoscopies performed among eligible individuals following a positive test and the percentages of individuals for whom the CRCDC was able to obtain a final diagnosis are factors influencing the recording of these lesions and may help explain departmental disparities. The definition of advanced adenomas, as defined in the “Guide to Data Format and Definitions of National Program Evaluation Indicators” and as recommended at the European level, aims to assess the proportion of lesions at high risk of malignant transformation. These are adenomas 10 mm or larger and/or presenting a villous or tubulo-villous component and/or having high-grade dysplasia. This definition differs from the definition used for clinical follow-up after polypectomy, which aims to guide colonoscopic surveillance protocols, particularly regarding the timing of recall. The lack of intra- and inter-examiner reproducibility in the diagnosis of advanced adenomas may also help explain the regional differences in observed rates of advanced adenomas1.
Screening Test Performance
The positive predictive value (PPV) of a test is the probability that a person is actually diseased if their test is positive. It is calculated by dividing the number of detected lesions (advanced adenomas or cancers) by the number of people who tested positive and underwent a colonoscopy.
The PPV of the screening test for advanced adenomas is 31.0% and 7.8% for cancers. These PPVs are higher among men than among women (35.5% and 24.9% for advanced adenomas, and 8.5% and 6.8% for cancers, respectively). They vary by department. For advanced adenomas, the lowest PPVs are observed in the departments of Saône-et-Loire (18.1%), Haute-Garonne (19.2%), and Aisne (20.8%), while the highest PPVs are observed in Mayenne (40.3%), Gironde (37.4%), and Meuse (36.9%). For cancers, the lowest PPVs are observed in French Guiana (2.4%), Corsica (4.6%), and Eure-et-Loir (4.8%), and the highest in Haute-Loire (11.5%), Aveyron (10.9%), and Lot (10.6%).
Stages of Detected Cancers
The stage of cancers detected by the organized screening program was determined according to the international TNM classification of malignant tumors.² This classification allows cancers to be categorized based on their degree of anatomical spread: local (or T), lymph node (or N), and metastatic (or M) involvement. For the colon and rectum, it applies only to adenocarcinomas. For colon cancers, the histopathological pTNM classification was used. For rectal cancers, which may undergo neoadjuvant treatments prior to surgery—resulting in a change in the T, N, or M stage of the detected tumor—the quality of available data and the heterogeneity of methods for documenting staging information do not allow for the determination of the TNM stage prior to treatment. Consequently, only colon cancers (including the rectosigmoid junction) and rectal cancers that did not receive neoadjuvant therapy were included.
The cancer stage is considered unknown when at least one of the T, N, or M values is unknown (unless pT=Tis, in which case the TNM stage is in situ, or if M=M1, in which case the TNM stage is IV). Among the adenocarcinomas of the rectum (without neoadjuvant treatment) and colon detected, this information is missing in 35.8% of cases. When the stage cannot be determined, T is missing in 18.5% of cases, N is missing in 21.6% of cases, and M is missing in 34.1% of cases. This percentage of adenocarcinomas of unknown stage reveals significant regional variation: it ranges from 0.4% to 100% (table in xlsx and pdf formats), as information on the metastatic status of detected cancers is difficult to access.
The description covers only the 44 departments with less than 30% missing data on cancer stages, corresponding to 7,980 detected colorectal adenocarcinomas (without neoadjuvant therapy). Among these adenocarcinomas, 10.3% are of unknown pTNM stage.
Among adenocarcinomas with a known stage, 32.3% are carcinomas in situ and 67.7% are invasive cancers (stages I to IV), of which 45.7% are stage I, 22.8% are stage II, 23.0% are stage III, and 8.5% are stage IV (table in xlsx format and pdf format).
1 Denis, B., Bottlaender, J., Breysacher, G., Chiappa, P., Peter, A., Weiss, A.-M. The advanced adenoma: A topical concept but an outdated definition? (2011) Hepato-Gastro, 18 (3), pp. 269–276.
2 Sobin M, Gospodarowicz L, Wittekind C. (eds). International Union Against Cancer. TNM Classification of Malignant Tumors, 7th Edition. Chichester: Wiley-Blackwell; 2009. 310 pages.