Epidemiological characteristics of botulism in humans in France in 2017
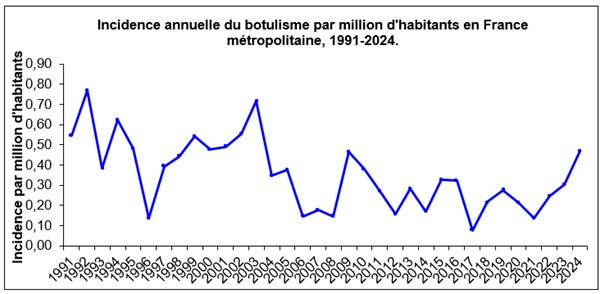
In 2017, four outbreaks of botulism were reported in France, involving a total of five cases (Figure 1). One outbreak occurred in a household setting.
The incidence rate of botulism was 0.08 per million inhabitants. This rate is significantly lower than the average incidence rate observed for the period 1991–2016, which was 0.37 per million inhabitants per year.
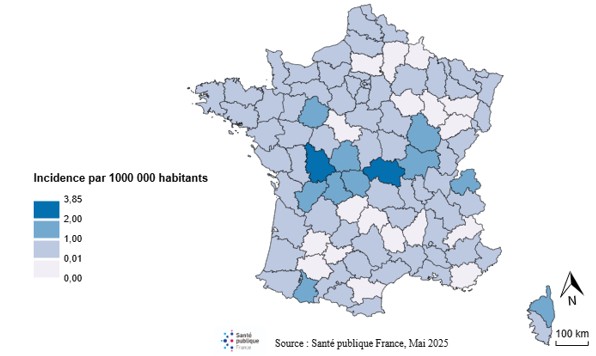
Since 1991, the highest average annual incidence rates have been observed in the departments of Vienne (3.9/106), Allier (3.1/106), Indre (1.9/106), Saône-et-Loire (1.9/106), and Creuse (1.8/106) (Figure 2). The high incidence observed in Haute-Corse (1.7/106) is attributable to a family foodborne illness outbreak involving five cases that occurred in 2010.
Analysis of botulism incidence by department reveals that the departments most affected by this disease during the 1991–2017 period are concentrated in the center of the country. It also shows that the majority of departments have been affected by the disease at least once since 1991 (Figure 2).
For 1 of the 4 outbreaks reported in 2017, a foodborne origin was confirmed; the source was a commercially packaged, vacuum-sealed dish of soy meatballs that had been consumed after its expiration date.
Consumption of a homemade hare terrine was reported in connection with another outbreak (2 cases) but could not be confirmed due to the lack of food remnants for analysis.
One case of infant botulism occurred, with no indication of consumption of a high-risk food. A possible environmental source could not be confirmed by analysis of household dust.
For the suspected case of botulism, a commercially prepared infant food product stored under poor conditions is suspected of causing the symptoms, with a significant presence of gas-producing anaerobic bacteria in the unconsumed jars that were analyzed.
The diagnosis of botulism was confirmed for 3 of the 4 outbreaks, with the presence of type B toxins in all 3 outbreaks.
Of the 5 patients identified, 4 were men, and the median age was 21 years. Two outbreaks occurred in January, 1 in February, and 1 in November.
A summary of the foods implicated as the source of the 2 confirmed outbreaks of foodborne botulism and the results of food samples are presented in Table 1.
Food samples were collected for 2 of the 3 outbreaks where a food of concern was identified: for one of these 2 outbreaks, a strain of C. botulinum type B was found in the food (vacuum-packed soy meatballs); the food analysis for the second outbreak was negative.
For the outbreak without food remnants, consumption of hare terrine was suspected to be the cause of the botulism cases.
For the confirmed infant botulism outbreak, an environmental source was suspected, but analysis of household dust did not reveal the presence of Clostridium botulinum spores, and the cause of this case remains unexplained.
| Type of toxin: human samples | Food in question (manufacturing) | Food sample result (toxin; C. botulinum strain) |
|---|---|---|
| B | Industrially produced soy meatballs (vacuum-packed) | B;B |
| B | Hare terrine (homemade) | No sample taken |
| Baby food jars (commercial) | No sample taken |
In conclusion, the number of botulism cases reported in 2017 was significantly lower than the median annual number of cases (N=23) reported during the 1991–2016 period. The number of botulism outbreaks reported in 2017 (4) is also lower than the median number (N=13) of annual outbreaks during the 1991–2016 period.
Type B botulism, primarily associated with deli meats, remains the most prevalent type of botulism in France. Although the vast majority of botulism cases are linked to foods traditionally considered high-risk, it remains important in any botulism case—particularly when no food traditionally associated with botulism risk has been identified—to consider other foods that could be potential sources of botulism poisoning (1).
Data from the 2017 botulism surveillance program highlight the need for continued vigilance regarding human botulism in France in order to monitor its trends and adapt prevention and control measures as necessary.
References
1-Tréhard H, Poujol I, Mazuet C, Blanc Q, Gillet Y, Rossignol F, Popoff M, Jourdan Da Silva N. A cluster of three cases of botulism caused by Clostridium baratii type F, France, August 2015. Euro Surveill. 2016;21(4):pii=30117.