Hepatitis A in France. Epidemiological data for 2022–2024.
Access the summary of hepatitis A surveillance data in France from 2022 to 2024.

Hepatitis A
thematic dossier
Hepatitis A is a waterborne disease with humans as its reservoir, and it can be prevented through vaccination. The hepatitis A virus is present in France and generally causes “sporadic” infections or outbreaks of limited scope due to adequate hygiene conditions across most of the country. Acute hepatitis A is a notifiable disease to enable the implementation of management measures for each diagnosed patient, particularly by offering vaccination to close contacts and recommending increased vigilance regarding adherence to simple hygiene measures such as handwashing.
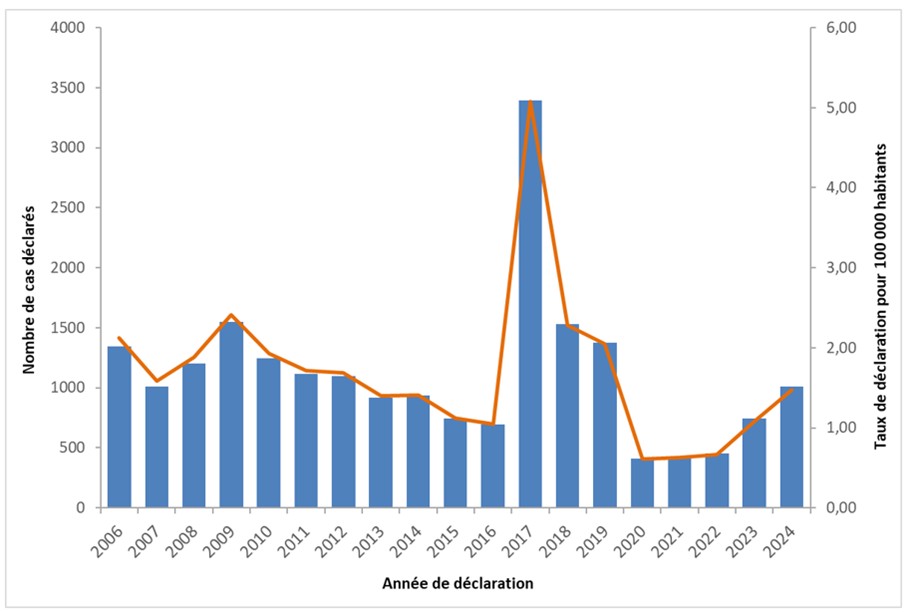
The reporting rate for acute hepatitis A in France has fluctuated since the implementation of mandatory reporting in 2006. A downward trend was observed between 2009 and 2016, with rates falling from 2.4 to 1.0 per 100,000 inhabitants. However, two notable events have influenced the epidemiology of hepatitis A in France since then:
In 2017 and 2018, a large-scale outbreak primarily affected men who have sex with men in Europe and France, with a reported rate reaching 5.3 per 100,000 inhabitants and 3,391 cases in 2017
In 2020, the COVID-19 pandemic led to a significant decrease in international travel and the implementation of preventive measures, including handwashing in particular. This resulted in an unprecedented drop in the hepatitis A case rate, which fell to 0.61 per 100,000 inhabitants with 411 cases reported in 2020
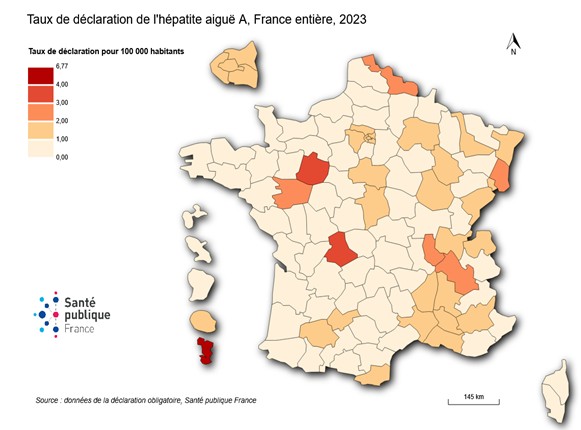
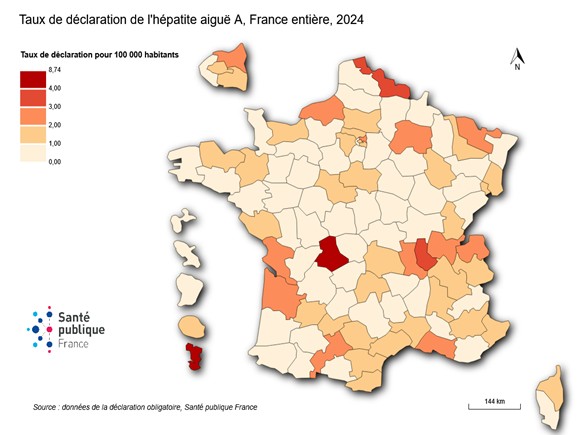
Since 2021, the number of reported cases of acute hepatitis A has been gradually increasing. It remained low in 2022 with 451 cases (compared to 423 in 2021 and 411 in 2020), corresponding to a reporting rate of 0.66 per 100,000 inhabitants. In 2023 and 2024, the reporting rate increased to 1.09 and 1.48 per 100,000 inhabitants, respectively, representing 742 cases in 2023 and 1,010 cases in 2024.
The low incidence rate still observed in 2022 was no longer linked, as in 2020, to a lower proportion of cases associated with international travel, since this proportion had returned to pre-pandemic levels (46.7%, as in 2019) (Figure 4). This continued low incidence was likely due to reduced international circulation of the virus and the continued implementation of preventive measures, such as hand hygiene, promoted as part of the response to the COVID-19 pandemic. In 2023 and 2024, the gradual phasing out of preventive measures likely contributed to the resurgence of acute hepatitis A cases in France, as well as that of other communicable diseases (measles, pertussis, invasive meningococcal infections, etc.).
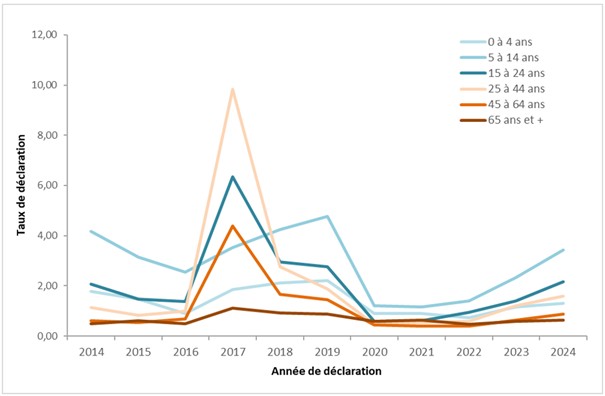
Between 2022 and 2024, the male-to-female sex ratio was 1.2 (compared to an average sex ratio of 1.3 between 2006 and 2016, and 3.6 in 2017*). The average annual case rates were 1.2 per 100,000 population among men and 1.0 per 100,000 population among women. The average age of reported cases was 33 years in 2022, 31 years in 2023, and 30 years in 2024. Report rates per 100,000 inhabitants by age group were highest among those aged 5 to 14 (1.4 in 2022, 2.32 in 2023, and 3.43 in 2024) and among those aged 15 to 24 (0.5 in 2022, then 0.6 in 2023 and 2024), as is typically observed (with the exception of 2017).
Between 2022 and 2024, jaundice was reported in the majority of reported cases (72%), and more than half were hospitalized (54.1%). This high hospitalization rate could be linked to more comprehensive reporting in hospital settings compared to private practice, or to reduced use of outpatient care for mild symptoms—though it is not possible to determine this with the available data.
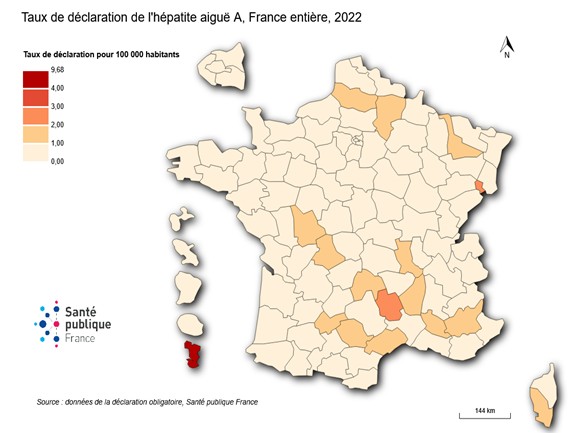
Regarding geographic distribution, as in previous years, the majority of cases were reported in mainland France, particularly in the Île-de-France region; however, the highest reporting rate was observed in the overseas department of Mayotte (9.7 per 100,000 inhabitants in 2022, then 6.8 in 2023, and 8.7 in 2024).
Between 2022 and 2024, the main risk exposures reported in the 2 to 6 weeks prior to the onset of symptoms were consistently:
A trip abroad (without it being possible to confirm that the infection was imported), which has been increasing since 2022, reaching 52% of cases in 2023 and 2024
Contact with a case in the immediate circle (in 25% of cases in 2022, then 33% in 2023 and 2024)
Consumption of seafood (22% in 2022, and 18% in 2023 and 2024), although it is not possible to confirm foodborne transmission based on the available data
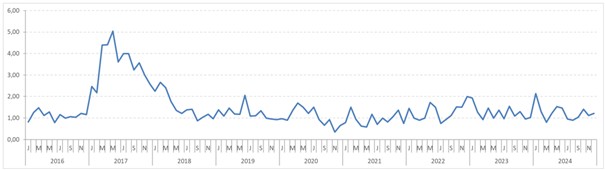
In 2022, 2023, and 2024, the typically strong seasonality in case numbers (namely, the significant increase in reports in September and October following trips to endemic areas during summer vacations) was observed again, reaching levels similar to those in the years prior to the COVID-19 pandemic.
A few small clusters of acute hepatitis A cases led to management measures between 2022 and 2024, such as clusters linked to schools, child care providers, or caterers. An outbreak limited in number of cases, linked to the consumption of oysters farmed in Normandy, also occurred in April 2024, with about twenty reported cases sharing the same epidemic strain and possible exposure to these oysters.
In conclusion:
Four years after the onset of the COVID-19 pandemic, the epidemiology of hepatitis A has returned to its usual characteristics in terms of demographic distribution, the populations most affected, and reported exposures.
Prevention Measures
To limit the spread of acute hepatitis A, vaccination recommendations remain in effect, advocating for increased vaccination among MSM following the 2017 outbreak, as well as among family members of a confirmed case, and during travel to areas with moderate or high endemicity (Vaccination Schedule and Recommendations for Travelers). Adherence to personal and public hygiene, particularly frequent handwashing with soap and water, also remains essential to limit the risk of hepatitis A transmission.