Outbreaks of foodborne illness suspected to be linked to the consumption of oysters contaminated with norovirus
Several outbreaks of foodborne illness potentially linked to the consumption of contaminated oysters have been reported since mid-February 2021 in several regions of France.

Outbreaks of foodborne illness
thematic dossier
A foodborne illness outbreak is defined as the occurrence of at least two cases with similar symptoms—typically gastrointestinal—that can be traced to a single food source. In France, such...
Update as of March 4, 2021, on reported foodborne illness outbreaks
Since mid-February 2021, 46 mandatory reports (DO) of collective foodborne illnesses (TIAC) suspected to be linked to the consumption of oysters have been submitted to Santé publique France and/or the Directorate General for Food.
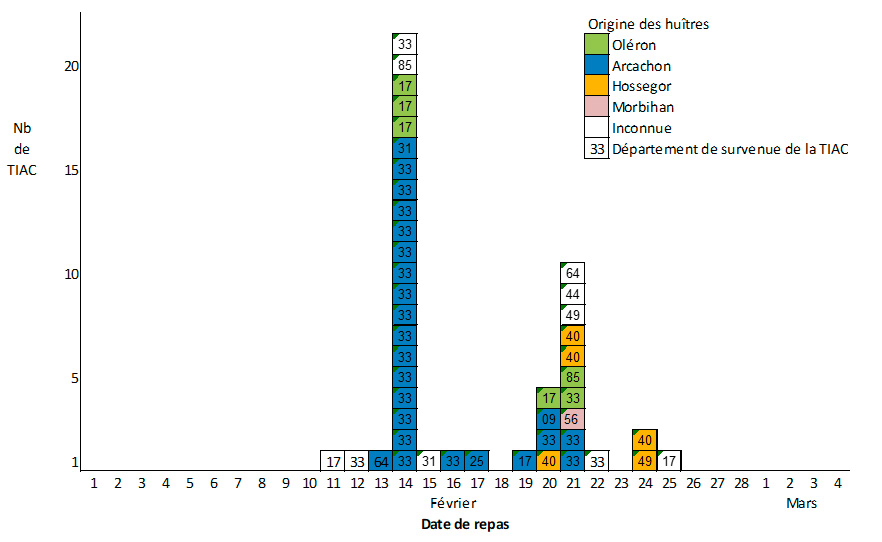
The dates of the meals associated with these foodborne illnesses range from February 11, 2021, to February 25, 2021, with the majority of cases reported on February 14 (21 outbreaks, 46%). All of these foodborne illnesses occurred during family meals involving between 2 and 8 people. A total of 164 cases were recorded, and two people were hospitalized.
Several departments were affected, particularly in the West region
Most of these foodborne illnesses occurred in Nouvelle-Aquitaine (23 in department 33, 7 in 17, 4 in 40, and 2 in 64), 5 in Pays de la Loire, 3 in Occitanie, 1 in Brittany, and 1 in Bourgogne-Franche-Comté. For 36 of these foodborne illness cases, the origin of the oysters is known: Arcachon Bay for 24 cases, Lake Hossegor for 5, Marennes-d’Oléron for 6, and Plouharnel Bay for 1.
Investigations conducted
Stool analyses conducted by the National Reference Center for Gastroenteritis Viruses in patients following two foodborne illness outbreaks confirmed the presence of norovirus.
Shellfish samples collected from individuals who became ill after consuming oysters, as well as from suppliers, were analyzed by reference laboratories and laboratories accredited by the Ministry of Agriculture and Food: noroviruses were identified. Noroviruses were also detected in several production areas of the oysters consumed.
Norovirus contamination of shellfish is also suspected for the other foodborne illness outbreaks, given the symptoms of those who fell ill—primarily diarrhea and vomiting—and the incubation periods between shellfish consumption and symptom onset identified during the investigations of the foodborne illness outbreaks. The torrential rains observed in early February may have contributed to the contamination of the environment/production areas and, consequently, the shellfish.
Measures taken since the detection of cases
Four areas are currently closed by prefectural orders imposing a temporary ban on the fishing, harvesting, transport, purification, shipment, storage, distribution, sale, and consumption of shellfish following the discovery of norovirus contamination in shellfish: the Arcachon Basin (Gironde) since February 18, 2021, Lake Hossegor (Landes) since March 2, 2021, the Chenaux du Payré (Vendée) since February 25, and Plouharnel Bay (Morbihan) since March 3, 2021.
Learn more: http://www.atlas-sanitaire-coquillages.fr/ (See the “Statutes” section)
What is a foodborne illness outbreak?
A foodborne illness outbreak is defined as the occurrence of at least two cases of illness with similar symptoms, typically gastrointestinal, where the cause can be traced to the same food or meal. Anyone (doctor, manager of a food service establishment, consumer, etc.) who becomes aware of an incident that may be a foodborne illness outbreak must report this suspected outbreak to the relevant authorities (Regional Health Agency (ARS) and/or the Departmental Directorate for Social Cohesion and Population Protection (DD(CS)PP)). This report triggers notification of the other agency (ARS or DD(CS)PP) at the local level. Joint investigations are then conducted to confirm that it is indeed a foodborne illness and to identify the contaminated food in order to implement the necessary preventive and corrective measures.
What is gastroenteritis?
Gastroenteritis is an inflammation of the intestines and stomach caused by microbes, which may be bacterial or viral in origin, or, more rarely, parasitic. Winter gastroenteritis is primarily viral in origin, with norovirus and rotavirus being the most common. After an incubation period ranging from 24 to 72 hours, it manifests as diarrhea and vomiting, which may be accompanied by nausea, abdominal pain, and sometimes fever. The illness is generally short-lived, lasting only a few days. The main complication is acute dehydration, which most often occurs in the very young and the very old.
Winter is the season with the highest risk of viral gastroenteritis, which is primarily transmitted from person to person (through dirty hands). However, these viruses, particularly noroviruses, can also be transmitted through food by ingesting water or food that is consumed raw or undercooked. These foods are contaminated either by a person carrying the virus during meal preparation or during production through contact with water contaminated by feces (e.g., oysters, berries, etc.).
Prevention tips to limit the spread of gastroenteritis viruses to those around you
Gastroenteritis is contagious, especially when caused by a virus. To limit its spread to those around you, follow these hygiene precautions.
Hands are a major vector for the transmission of acute viral gastroenteritis. To reduce the risk of transmission, wash your hands frequently (before preparing meals, before eating, after using the restroom or caring for a sick person or changing a baby, after being outside, etc.).
Clean the toilet with a disinfectant after each episode of diarrhea or vomiting.
Since certain viruses (rotavirus and norovirus) are highly resistant in the environment and can be found on surfaces, frequently touched surfaces such as doorknobs, the telephone, toilets, and sinks should be cleaned more frequently and thoroughly if you or someone in your household has diarrhea or vomiting.
Paper towels should be changed regularly.
People with diarrhea or vomiting should avoid helping to prepare meals.